Last week I posted about the new CDC school guidelines. I mentioned that there were two major gaps in the scientific literature:
Operationalizing the risk of teachers when schools are NOT opened safely
Operationalizing the risk of of people living with teachers and students
Well…I spoke too soon; this week two studies came out answering these very questions (at least to some extent).
The first was a CDC study conducted in 8 public elementary schools in a single Georgia school district. From Dec 1, 2020–Jan 22, 2021, the local health department contact traced anyone at the schools who tested positive for COVID19. During this time, 2,600 students (approximately 80% of students) and 700 staff members attended school in person. It’s important to note that at this time COVID-19 transmission in the community was high (increased almost 300% during the study period). This is what the scientists found…
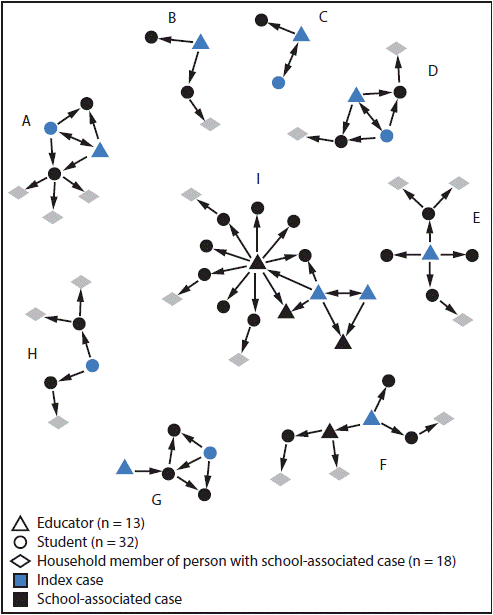
There were 9 COVID19 clusters during this time period in 6 (of the 8) schools. The clusters involved 13 teachers and 32 students
Of the 9 clusters, index cases (those that started the disease clusters) were:
4 teachers
1 student
4 couldn’t be determined
Of the 9 clusters,
8 involved at least one teacher
8 involved teacher-to-student transmission
4 involved student-to-student transmission
3 involved student-to-teacher transmission
2 involved teacher-to-teacher transmission during meetings or lunches, which was followed by educator-to-student transmission in the classroom and resulted in 48% of cases
26% of household members were infected because of the 9 clusters
Of the 9 clusters,
7 occurred during small group instruction sessions in which teachers worked in close proximity to students
5 clusters were due to lack of or inadequate mask use by students likely (students ate lunch in their classrooms, which might have facilitated spread).
The second “study “ described student and teacher ICU admissions in Sweden. It wasn’t really a study but a “correspondence” in the New England Journal of Medicine. Sometimes correspondents are peer-reviewed but sometimes they are not (just depends on the journal). What did the authors report?
The scientists described data from March through June 2020 in Sweden on Covid-19 among children 1 to 16 years of age and their teachers. Remember, Sweden was one of the only countries that did NOT institute strict lockdowns like the U.S. (at least in the beginning of the pandemic; they had to change strategies once deaths began to exponentially increase). This is what the scientists reported…
A total of 15 children with COVID19 were admitted to an ICU (0.77 per 100,000 children) during this time period. No child with Covid-19 died
A total of 10 preschool teachers and 20 schoolteachers with COVID19 were admitted to an ICU (this equates to a risk of 19 per 100,000 school teachers)
Risk of COVID19 ICU admission was lower for school teachers compared to other professions
Bottom line: This (finally) starts to close our knowledge gap on the risk to teachers and risk to family members related to teachers/students. If there is a COVID19 cluster (which is relatively rare), teachers are touched. Also, transmission from teacher-to-teacher, teacher-to-student, and student-to-student exists when public health measures are not in place (especially during lunch or meetings). This transmission is then brought home.
We need a whole lot more data (especially among high schools) to make sweeping policy decisions, but nonetheless an important glimpse into school transmission.
Love, YLE

Thank you! As the wife of an elementary educator (in class 4 days, in building 5) and mom of 3 children who are in class 2 days a week this information is appreciated.
Slightly off topic, but could you explain the surge you’re expecting in March?
Selfishly I want to know because our school district is currently phasing in from virtual to hybrid learning. Then they’ll monitor the data for March to decide if/when to go back to fulltime. But if there’s a surge in March I’m afraid they’ll send us all back to virtual.