By now we know that mortality is not the only outcome of COVID-19 disease. The virus can reach all of our organs, so a number of survivors continue to battle symptoms long after initial disease.
How does SARS-CoV-2 reach organs?
We have COVID19 doors (called ACE2 receptors) on almost all of our organs. The little spikes on the virus are keys to these doors. It takes about 10 minutes for COVID19 to open the door and make a cell its home. Once in, the virus starts multiplying eventually killing the cell (and sometimes even killing all the cells in the organ). On top of this, our immune system then “overreacts” to these cells dying causing even more problems. This has been documented to happen in almost every organ in the human body, even among those with asymptomatic disease.
Including the brain
Our brains are highly protected, so we aren’t entirely sure how the the virus enters the brain yet. One strong hypothesis is that invasion happens at nose cells and then progresses from there onto a region at the front of the brain (called the olfactory bulb responsible for smell). In the short-term, the virus causes inflammation of the brain. The brain can also be indirectly impacted by blood clots or lack of oxygen.
There can be neurological damage in the long-run too. Back in July 2020, JAMA published one of the first studies describing neurological symptoms long after initial disease. This was followed by a multitude of studies of patients reporting loss of smell and taste, headaches, and dizziness; 33% of patients experience neurological or psychological “COVID19 fog”; and, mental health issues lead to struggling for words, simple math, or just trying to think well after survival.
Brain Tissue
Just recently, a group of scientists at Oxford found that it might be because some survivors lose brain tissue. As part of an ongoing study, 782 volunteers’ brains were scanned 3 years before the pandemic. The same adults were then invited for a follow-up brain scan during the pandemic: 394 of them had survived COVID19 (ranging from asymptomatic to severe disease) and 388 never had COVID19.
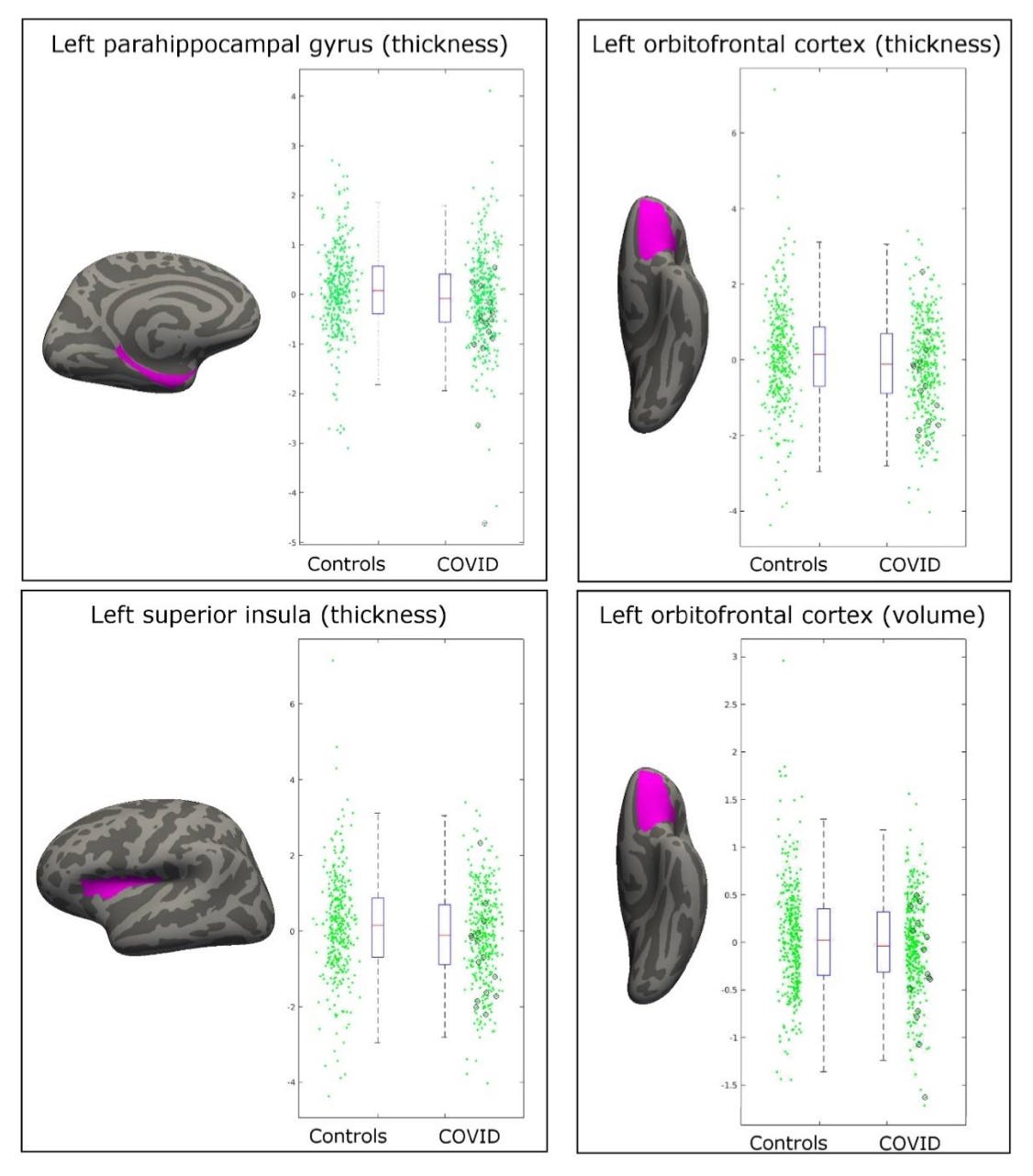
How did their brains compare? Those with COVID19 had significant loss of gray matter, particularly in three specific areas on the left side of the brain. This brain matter loss was regardless of disease severity. Those without COVID19 had no brain tissue loss.
Interestingly, these three regions of the brain are responsible for smell, taste, memory, and emotion. This could possible explain the long term neurological symptoms among COVID19 survivors.
Linked to Alzheimer’s?
Quite a few scientists are concerned that this may be setting up for Alzheimer’s in the future. As NPR reported, the Alzheimer's Association International Conference is meeting in Denver this week. At conferences, scientists present hot off the bench results. The results are not published and not even in pre-print, but still important because they give everyone an idea on what their working on, give a taste of preliminary results, and can spark conversations and collaborations.
As you can imagine, this year many scientists are presenting on their work in COVID19 and Alzheimers. Some preliminary presentations include:
Scans taken before and after a person develops COVID-19 suggesting that the infection can cause changes that overlap those seen in Alzheimer's
Genetic studies showing the same genes that increase a person's risk for getting severe COVID-19 also increase the risk of developing Alzheimer's
Mental problems being more common in COVID-19 patients who lose their sense of smell because the disease has affected a brain area
The link between Alzheimers and COVID19 isn’t too far fetched either. Previous research has shown how other viruses can increase the risk of Alzheimers and dementia.
Unfortunately, we’re at the mercy of time to see how this manifests, as there are still a lot of unanswered questions. If there is a true link between Alzheimers and COVID19 we think it will be relatively rare, but with a global pandemic, the population-level impact will be devastating.
Love, YLE





Fabulous.
This just gets worse and worse, doesn't it?
Katelyn, my deepest gratitude to you for your work.
Sending love right back to you.
Thank you for this! I'm pretty sure I somehow managed to contract COVID waaaay back in January 2020, as I had all the symptoms except for loss of taste and smell, the cough lingered for a good 6 or 7 months, and my lung capacity - already pretty crummy from asthma - never has fully recovered. I've also noticed since then that my usual knack for words fails me more and more often, but I hadn't thought to connect the two!
Also, potential brain problems are about the only risk that I think my dad might actually take seriously; especially after losing his mother to dementia last year. I forwarded your email newsletter to him, and described my own mental symptoms. Maybe it'll finally convince him to get vaccinated. *fingers crossed*