I’m getting many, many questions about another booster, including from my 90 year-old grandparents. Here are some answers.
What happened?
This week the FDA and CDC officially recommended the following:
mRNA series: A booster for certain immunocompromised individuals and people over the age of 50 who received an initial booster dose at least 4 months ago
J&J: All adults who received a primary J&J vaccine and booster dose at least 4 months ago may now receive a second booster dose using an mRNA vaccine
This is a clearly a proactive move as officials didn’t wait for the upcoming FDA meeting on April 6. Maybe because BA.2 is looming in the background? Nonetheless, the scheduled FDA meeting is still important as scientists will openly discuss the science, options, and long-term plan for COVID-19 vaccines in the U.S.
Should I get a fourth dose?
The original booster continues to do a great job at preventing hospitalization and death. There is some evidence that this is waning over time, though. Your decision should be driven by weighing benefits with risks:
Benefit: There is evidence from Israel (2 studies here, here) that shows a fourth dose provides additional protection for older adults. The benefit isn’t nearly as drastic as a third dose, but benefit is there. For example, among a sample of 1,138,681 Israelis aged 60+ years, a fourth dose reduced the rate of infection by 2 times and reduced the rate of severe disease by 4 times. Preventing infection will also reduce chances of long COVID.
Risk: The vaccine poses very, very low risks. Some people (like me) do experience side effects, which puts you out of commission for a few days. If you can’t miss work or don’t have sick time then this may outweigh the benefits for healthy individuals right now. (Although you would have to miss more work if you were infected.)
To me, the benefits of a fourth dose outweigh the risks, so I’m supportive of a fourth dose booster for those who are eligible.
We are clearly in a lull right now. Because antibodies wane, should I wait for the next wave and/or for fall?
A fourth dose can certainly be delayed. But there are a few challenges with this:
Timing is difficult. I would caution against trying to time a booster right before a wave. Like Dr. Bob Watcher said, it would be like trying to time the stock market. We know that this virus continues to mutate and a variant of concern could pop up. We also know that boosters take time to work to their full potential. Finding a timing sweet spot of boosting before a wave is possible, but potentially risky with not much added benefit.
Uncertain future. The current booster debate eerily reminds me of the booster debate last fall. Many scientists and clinicians said there wasn’t enough evidence for boosters. I even said: “I’m not convinced that I (a healthy, young person) needs it (…) but I will stand in line come September if it’s recommended.” But, boy, were we lucky to have boosters before Omicron arrived. Just like with last fall, we don’t know what the future holds. But we can prepare for the worst and hope for the best.
Next move after delaying. We will likely have a fall/winter wave given that coronaviruses thrive in winter. I’m hopeful that fourth dose boosters will be durable. If not, we may need another booster or an updated vaccine formula before winter. If you delay a fourth dose now, what should you do then? There’s considerable benefit to sticking to the recommended CDC schedule. The science and future recommendations won’t be following any other timeline. If you go rogue, future decisions may be difficult to navigate.
Do I need a booster if I was infected with Omicron?
If you had the first booster and a confirmed Omicron infection (i.e. positive antigen test or PCR test), there’s really very little need to get a fourth dose. Vaccine + infection is called “hybrid immunity” and over 20 studies have shown this works fantastic due to complimentary and broad protection: Vaccine immunity targets the spike protein and infection-induced immunity targets the whole virus. This doesn’t mean you should purposefully get COVID19, but we need to recognize this as a viable path to protection.
To be clear, the FDA and CDC do not recognize hybrid immunity as an option. So, if you don’t go off the official schedule and rely on hybrid immunity, then future moves, like when to get another vaccine, may be tough to navigate. Before Omicron, evidence found that hybrid immunity worked great for at least 1 year. (Omicron is probably negatively impacting this timeline a bit).
Which booster should I get?
Consider mixing your fourth dose. If you got three doses of Pfizer then get Moderna for your fourth dose. Or vice versa.
While Moderna and Pfizer are both mRNA vaccines, they are not identical and have subtle but meaningful differences. (See my previous post: Moderna vs. Pfizer: Is there a difference?)
This was confirmed yesterday from another peer-reviewed study. Scientists found that while the two different shots have the same impact on neutralizing antibodies, they have a different impact on Fc-functional antibodies, which target the whole surface of the spike protein. They also had a different impact on T-cell mechanisms. If you mix vaccines you have the potential to maximize protection.
Should you wait for an Omicron-specific booster?
We are still waiting on results from human studies, but two animal studies have shown that Omicron-specific boosters are not more effective than the original vaccine formula. One study randomly assigned primates to an Omicron-specific Moderna booster or regular formula booster. They found no difference in the rise in neutralizing antibody levels against any variants of concern. In other words, I wouldn’t hold your breath or delay for an Omicron-specific vaccine.
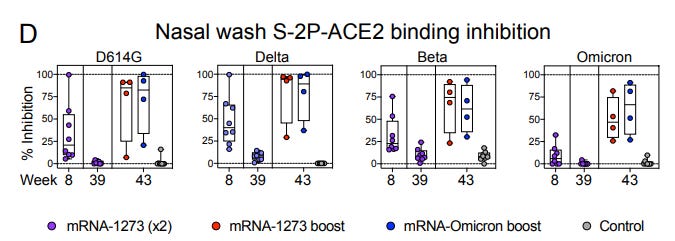
What changed with J&J recommendations?
A J&J+ 1 mRNA shot provides great protection. But a study published yesterday found that protection may be slightly less than the 3-dose mRNA series. Scientists found that while there was not a statistical difference in effectiveness against urgent care/emergency department visits, a 3-dose mRNA series had slightly higher protection against hospitalization. This evidence persuaded the CDC to recommend a second mRNA shot for J&J people.
Where can I find a vaccine near me?
There is a new government website called COVID.gov. It went live yesterday and is a one-stop shop for everything—current transmission levels (according to new CDC guidelines), vaccine and test & treat locations, ordering free antigen tests, etc. I’m incredibly impressed with the website and wish we’d had it throughout the entire pandemic. Here you can type in your zip code and find what vaccines are available where.
Bottom line
If you’re eligible, get your booster. Does a healthy 50 year-old adult need to rush and get one tomorrow? No. But I would put it on your to-do list. The older you are, the higher priority it should be on your to-do list. The future is uncertain, and the benefits of vaccines continue to outweigh the risks.
Love, YLE
“Your Local Epidemiologist (YLE)” is written by Dr. Katelyn Jetelina, MPH PhD—an epidemiologist, biostatistician, professor, researcher, wife, and mom of two little girls. During the day she has a research lab and teaches graduate-level courses, but at night she writes this newsletter. Her main goal is to “translate” the ever-evolving public health science so that people will be well equipped to make evidence-based decisions. This newsletter is free thanks to the generous support of fellow YLE community members. To support the effort, please subscribe here:




As a 74yo healthy physician I have gotten the 4th dose - the big motivator for me was the admittedly uncertain effectiveness of boosters to prevent or lessen impact of “long Covid”. From a quality of life perspective, that at this point is my big concern.
I'm an MD and read the linked article to support mix/match boosters-- and to my read it showed the better durability of Moderna vs Pfizer. So, I asked an ID colleague to double check and he agreed. He doesn't see the benefit of mix and match, unless you got Pfizer and can now get a Moderna. Just 2 MD's opinions. But I really respect the infectious disease doctor I consulted.