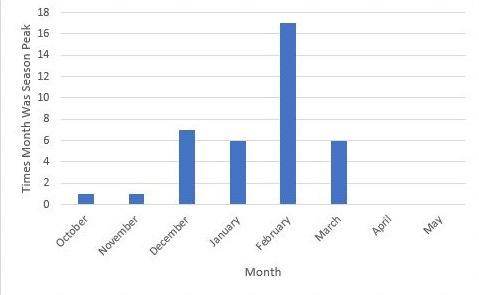
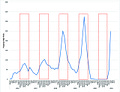
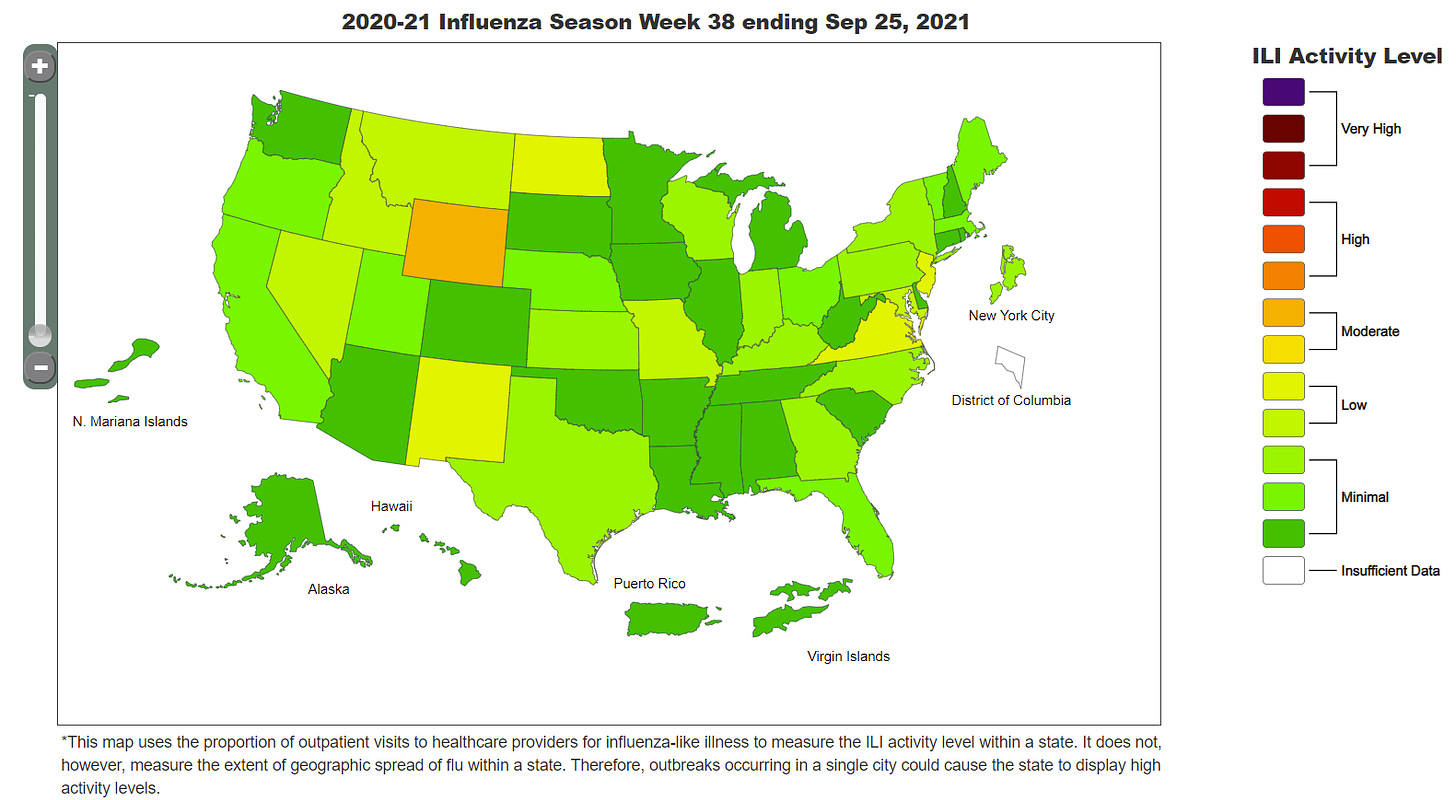
Flu (i.e. influenza) season is right around the corner. According to the CDC, only one state (Wyoming) has moderate influenza spread while the rest of the United States has minimal spread. While influenza is year round, flu activity typically peaks between December and February because of the colder weather and change in human behavior.
Vaccine Hesitancy
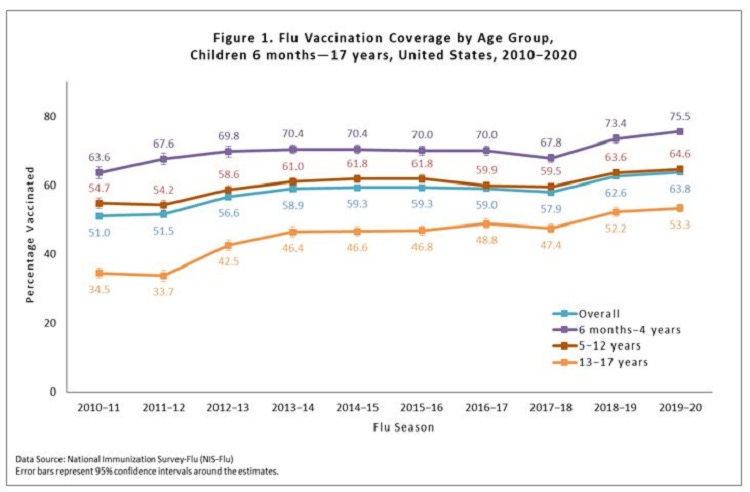
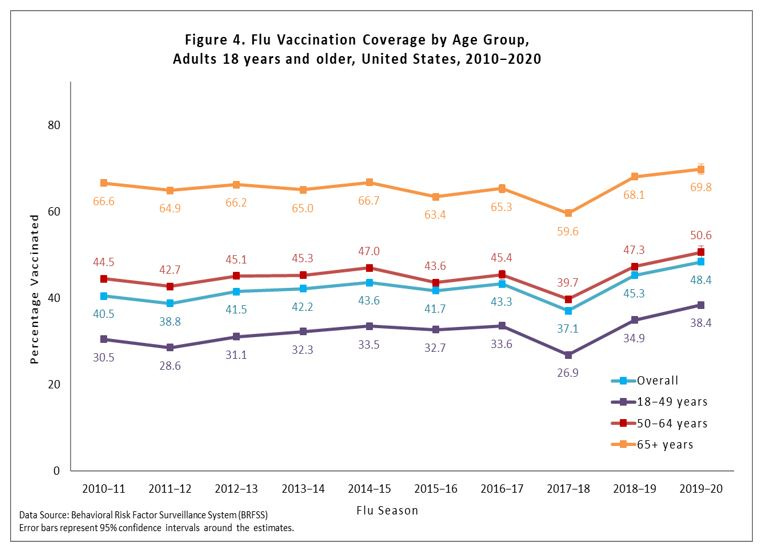
But Americans, and especially adults, notoriously skip the flu vaccine every year. During the 2019-20 flu season, 64% of kids and only 48% of adults were vaccinated for the flu. This year 60% of adults plan to get the vaccine (so far only 8% of Americans have the flu shot). And while this is a welcomed increase in vaccine uptake, more people should get in line.
Just like the COVID19 vaccine, there is a lot of flu vaccine misinformation (lack of knowledge, misperceptions, and distrust of vaccines). This causes suboptimal vaccine uptake each year. Some of the top concerns may sound familiar…
“I do not need the vaccination”. We have certainly normalized the flu than compared to, for example, COVID19. But that doesn’t make it any less serious. The overall burden of flu for the 2019-2020 was an estimated 35 million illnesses, 16 million medical visits, 380,000 hospitalizations, and 20,000 deaths. Influenza is the 9th leading cause of death in the United States (6th leading cause of death for 1-4 year olds).
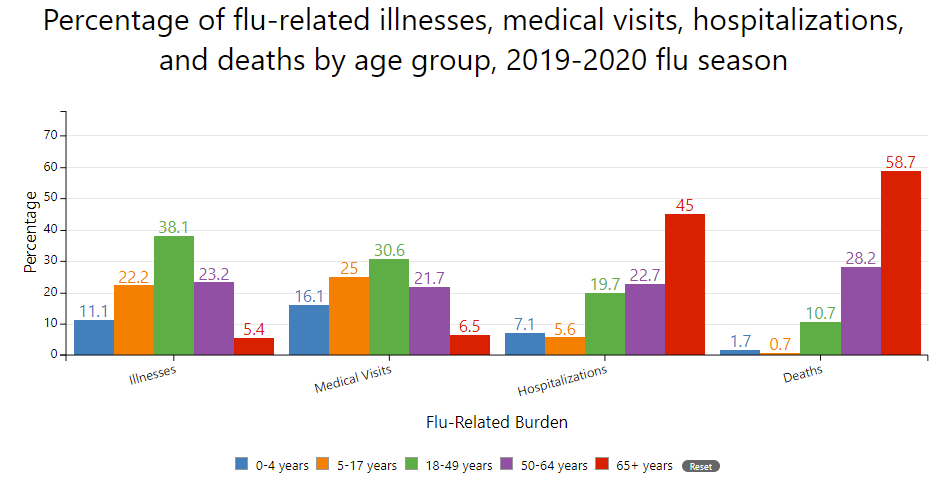
“I don’t think the flu vaccine works”. They actually work pretty well. The effectiveness is generally around 40-60%. During the 2019-2020 season, vaccination prevented 7.5 million illnesses, 3.7 million medical visits, 105,000 hospitalizations, and 6,300 deaths. And that was with only a 52% vaccination rate. If we got this higher, we could prevent a lot more. Among kids, a 2017 study found that flu vaccination reduced a child’s risk of dying in half.
“The flu shot can give me the flu”. This is biologically impossible as the shot does not have the live virus (the nasal spray does). A low-grade fever, headache and muscle aches may occur. But in randomized control studies the only differences in symptoms between vaccinated and the placebo was increased soreness in the arm and redness at the injection site among people who got a flu shot. There were no differences in terms of body aches, fever, cough, runny nose or sore throat. Nonetheless, side effects don’t last more than 24-48 hours. People also could just be unlucky and exposed to flu after vaccination but before the vaccine took effect. It takes about two weeks for the body to build protection against the flu.
“I got the flu shot last year, so I am protected”. You need to get a flu vaccine every year. Flu viruses are constantly changing (much faster than COVID19), so flu vaccines are usually updated from one season to the next to protect against the viruses research indicates may be most common during the upcoming flu season. Vaccine and/or natural immunity also wanes over time. Annual vaccination is needed for optimal protection.
“It’s too early for the flu vaccine”. October is actually the perfect time. A new study found a decline in vaccine effectiveness of about 8%–9% per month post-vaccination. Effectiveness wanes quicker among 65+ adults, so July or August is too early for a vaccine. It takes some time to mount a response, so it’s best to get the vaccine before flu activity starts.
The flu shot is especially important this year
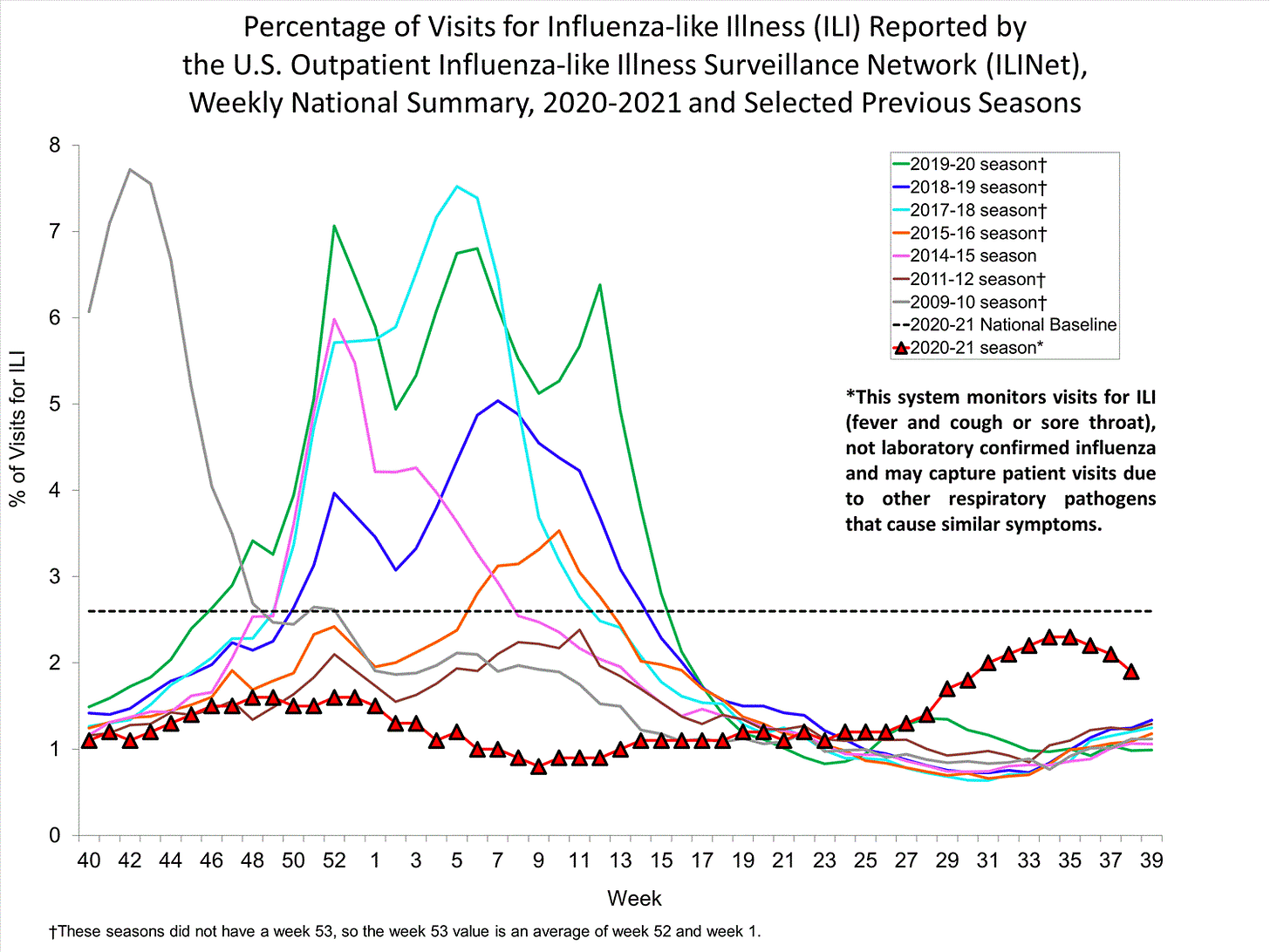
Influenza viruses circulated at historic lows last year due to the pandemic (masking, schools closed, no global travel). It was the lowest it’s been since 1996 (when we first stated tracking the flu). While a nonexistent flu season was a silver lining to the pandemic and necessary to curb COVID19 transmission, it may work against us this year.
Human immunity builds up over time. Because we’ve had prolonged absence of ongoing natural exposure to influenza viruses, our bodies may be surprised when we come in contact with the influenza virus this season. This is particularly true with kids under two that were born during the pandemic and never exposed to influenza.
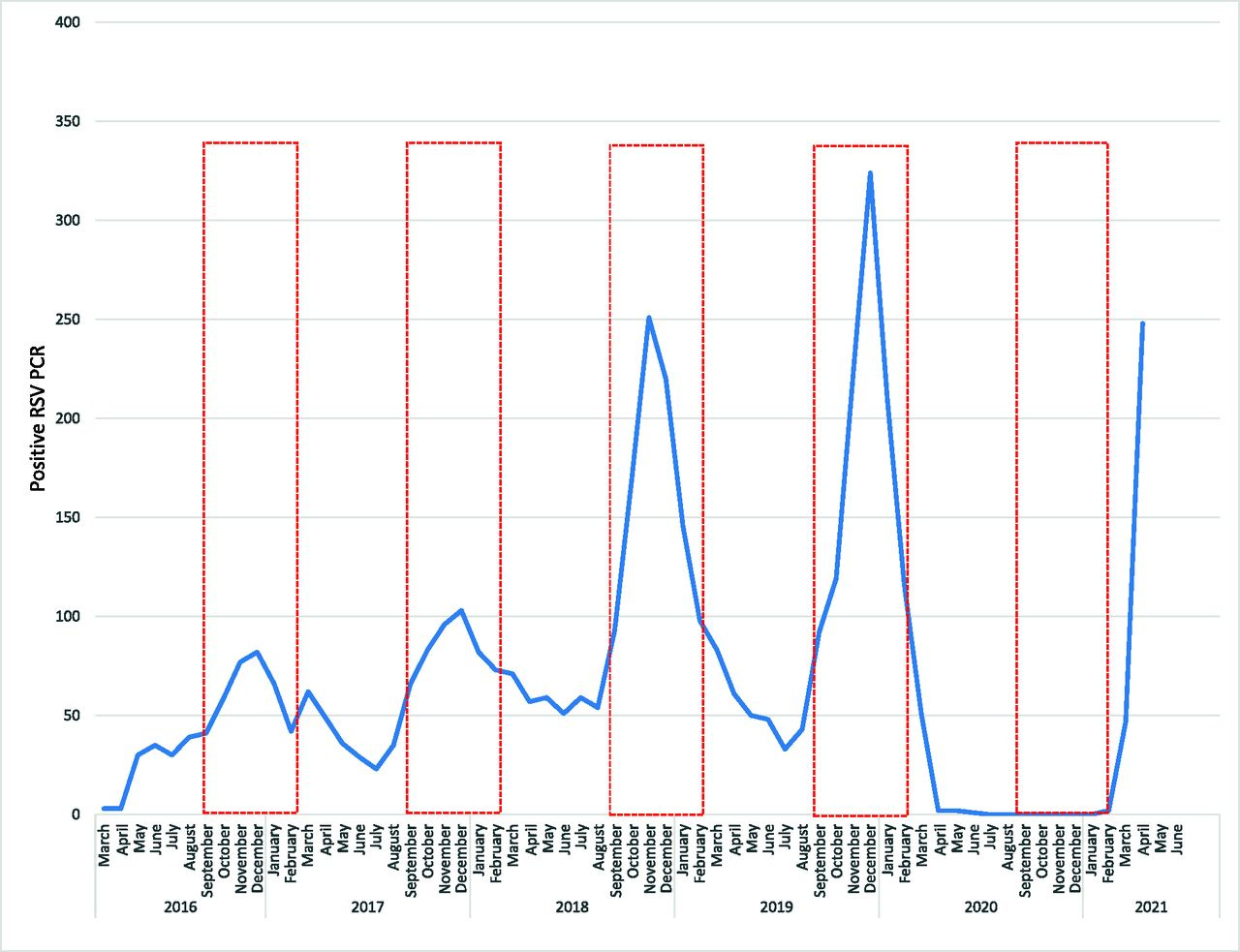
We got a preview with RSV (Respiratory Syncytial Virus). RSV can be serious for kids, especially those under 2, but it can also cause severe disease in adults too. This summer more and more people started taking off masks, traveling, and getting kids in childcare. This caused RSV to flare up at a very unusual time —summer— especially in the South. The first hospitalized RSV case was in March and, by July, in one week there were 2,000 confirmed cases recorded across the U.S. Data from a recently published Pediatrics article indicated more severe disease in younger infants because of diminished immunity from a lack of exposure to RSV in the previous season. The authors concluded:
“Institutions should plan ahead for an increase in pediatric emergency visits and, potentially, a need for increased PICU capacity in the coming weeks. Additionally, efforts should be made to extend monthly preventive palivizumab for infants at risk for severe RSV disease, to ensure continued protection during this unexpected surge.”
Added benefit? Flu vaccine may help protect against COVID19
An interesting preprint was released suggesting an added benefit to the flu shot: protect against SARS-CoV-2 infection. Dutch scientists conducted a large study among healthcare workers. They found that those with the flu shot were 47-50% less likely to get COVID19 than healthcare workers without the flu shot.
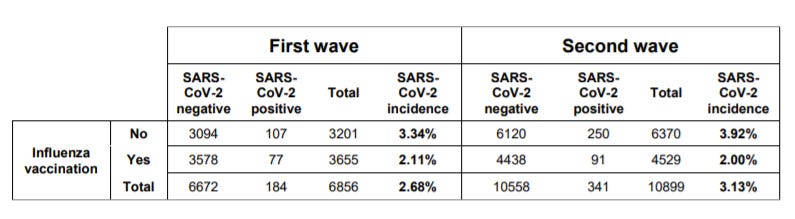
This is due to a phenomenon called “trained immunity”. While a flu shot isn’t nearly as effective as a COVID19 vaccine against COVID19, it may be an extra incentive for more hesitant parents to get their kids immunized against the flu this fall. Or other high risk groups, like pregnant people, who have yet to be inoculated against COVID19.
Bottom Line: Go get your flu shot.
Love, YLE


I was at the pediatrician yesterday, and he suggested that the low rates of flu in the last year would mean this year’s vaccine’s efficacy would be worse. His logic appears to be, since there was little flu circulating in the Southern Hemisphere to study, researchers wouldn’t be able to effectively anticipate what will be circulating here this season. Is there any validity to this?
I agree we should get our flu shots and I will too. A slightly alternative possibility I was hoping for is that the flu was given a massive knockout punch last year. For the first time in history the world did a massive shutdown right at the point where flu in the US is at its lowest point and on top of that a decline in travel slowed down the worldwide circulation of flu viruses. I have read they believe flu is actually extinct now in New Zealand and possibily Australia.
Likewise even today in the US we still have a lot of people avoiding indoors, using masks and the norm now is if you feel sick you stay home since going into school or work coughing, congested etc. is the best way to freak everyone out.
During my endless rhetorical battles with Covid truther types, I'm confronted with the "where did the flu go line". This is my standard answer, which no one ever seems to have a decent comeback against.
In this alternative I'm wondering if flu could be on the ropes for a long time before it comes back to where it was. Obviously if lots of people get vaccinated then that adds to the flu's woes in returning to its normal place. There is a possibility here the old models are not longer applicable because human behavior is not going to revert to the realitively innocent and unaware pre-2019 era.