Herd immunity is not a light switch
Yesterday, in my home city, health officials claimed victory in a news article entitled “Dallas County Reaches Herd Immunity Against COVID-19”. The article explained that 80% of the County had either previously contracted COVID19 and/or had received at least one vaccination.
This is exciting. (Although I would be more excited if vaccinations were accounting for this protection. We’re only 44% vaccinated). Maybe this means there’s light at the end of the long, pandemic tunnel. I can’t help but also track our immunity wall. It gives a sense progression.
However, we cannot come to erroneous conclusions once we reach a magical number in our head or on a county dashboard.
Herd immunity 101
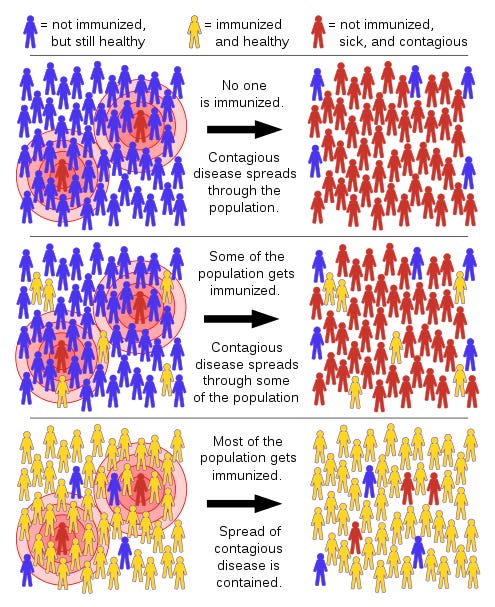
I think we all know by now that not 100% of our population has to be immune for COVID19 to wither away. We can get to a point where so few people have COVID19 that even those who can’t be protected (like the immunocompromised ) will never have the chance to get sick. An immunity wall will keep any outbreak or transmission from happening.
On a global stage, we’ve only hit herd immunity once. In 1980, the World Health Assembly declared that smallpox was eradicated thanks to a very successful global vaccination campaign. No cases of naturally occurring smallpox have happened since.
In 2000, the CDC also declared that measles was eradicated in the United States as we reached herd immunity. This was a huge achievement given that the measles is incredibly contagious; we needed ~95% herd immunity threshold. Unfortunately, this is not still the case. Because of the antivaxx movement, we continue to dip below the threshold of protection and outbreaks happen all the time. The 2019 measles outbreak at Disneyland is just one example.
Herd immunity threshold is really complex to measure.
We don’t even know what the magic number is for COVID19. In the beginning, scientists estimated a 69.6% threshold was needed to reach herd immunity in the United States. This was based on a lot of mathematical models and educated guesses. Importantly, this guess relied heavily on R(0).
But the pandemic is not a fixed. It continuously evolves. Which means this threshold continues to move. The more transmissible the variant (like Delta) the higher the threshold we need. Our behaviors also impact the threshold. Not wearing masks, not social distancing, etc. will also move our threshold higher. Population density, genetics, environment, and a whole lot of other things can also impact this number. Thus, herd immunity in the United States can be very different than what is needed in Canada. Because of this, it’s really difficult (in fact I would argue impossible) to forecast an accurate number.
Even if we knew the number, it’s not a light switch.
It’s not a finish line. Not a binary decision. Not a static goal post that, once we reach, this nightmare will end and everyone’s risk for COVID19 will be zero.
My friend and colleague, Dr. Malia Jones, explained what it might look like instead:
“(A) receding tide. As more and more people are vaccinated, those who are at highest risk for ending up in the ICU will be protected. We’ll all have growing protection from outbreaks as people who are high transmitters get vaccinated. (Looking right at you, young adults.) Cases will start to ebb overall, but we can expect some ups and downs. There will be more variants, and there will be more surges. We’ll have low enough transmission that we will be able to resume most normal activities.”
And herd immunity is not a city, county, or even state level metric.
The 80% threshold that Dallas reached is a pooled estimate. There are still significant pockets within Dallas that remain extremely vulnerable. Even though Dallas reached “herd immunity”, cases continue to rise in Dallas.
But even if there weren’t pockets within, viruses don’t see city lines. We live in a very transient and fluid society. We move between counties, states, and countries.
And it’s dangerous to think that viruses see lines. There’s a very real possibility that people will think they’re protected if we reach a magic number. They may wrongly think this is over, that vaccines aren’t important anymore, and that we can put our guard down. This is a dangerous game to play.
We may not reach herd immunity. But it isn’t all for nothing.
We don’t need to reach herd immunity for a pandemic to end; for us to reach some sort of pre-pandemic normality. Herd immunity is not a number we need for cases to all of a sudden plummet. Instead it’s a number we need in order to keep cases down AFTER they are already down. Like Dr. Jones says, it’s a policy goal.
During a Stanford panel, a number of experts agreed that the next phase will be an endemic: “a plateau in infection, with a decrease in prominence over time but continued circulation.” This will be a mild state in which we don’t have exponential swings but, instead, people will get sick on occasion.
Bottom Line
There is not going to be a “herd immunity day” where life immediately goes back to normal. We need to start thinking of it as a receding tide rather than a light switch. Yes, we should celebrate vaccine progression. And yes, some are still hopeful that we will eventually reach herd immunity. But it will be slow. It will be quiet. And we will only know we reached it until it’s passed.
Love, YLE