There are 14.6 million people in the United States left in the dark about their Johnson and Johnson (J&J) shot. Does it work against Delta? Is it safe and effective to get a second J&J shot? Can J&J folks mix shots? If so, which mix is the best?
We don’t know much and I’m incredibly frustrated about this. The lack of guidance or just plain communication from the private (J&J) and/or public sector is unacceptable.
I put together this post based on all the evidence we have today. I realize it’s data heavy, but I wanted to be sure you had a clear understanding of what we have and don’t have so you can make a data-driven decision. I also (reluctantly) provided some insight on what I would do if I had J&J…
Pre-Delta
Before Delta, J&J was doing fantastic. In the U.S. clinical trials, there was a 72% efficacy rate against infection. There was a 100% efficacy against hospitalization and death. In the real world, we saw an effectiveness of 76.7%. And, they seemed to hold up against previous variants (although we are still a bit worried about Beta).
Delta Infection
Then Delta came. We needed to quickly assess how well our vaccines (including J&J) were working. But, the U.S. doesn’t have the public health infrastructure to watch this in real time. We are reliant on other countries, like the UK and Israel, that do have these systems in place. Unfortunately, these countries don’t use J&J. So we were/are flying blind.
On July 2, J&J announced that their one dose regimen worked against Delta. Scientists took blood samples from 8 of their clinical trial participants. Then, in petri dishes, they infected the blood with Delta. (I reviewed the study in detail before here).
There was a 1.6-fold decrease in neutralizing antibodies. This is a very little decrease, which is great news. This means that the vaccine could still protect against Delta.
The problem was this is only 8 people. And this was a petri dish study. How did the vaccine work in the “real world”?
Delta Hospitalization
South Africa answered this question on August 7 when Glenda Gray, the president of the South African Medical Research Council and co-leader of the trial in a YouTube broadcast. There were 477,234 vaccinated healthcare workers who received the J&J vaccine in South Africa. Scientists looked at how the vaccine was holding up against Delta. What did they find?
91-96% protection against death
71% protection against hospitalization
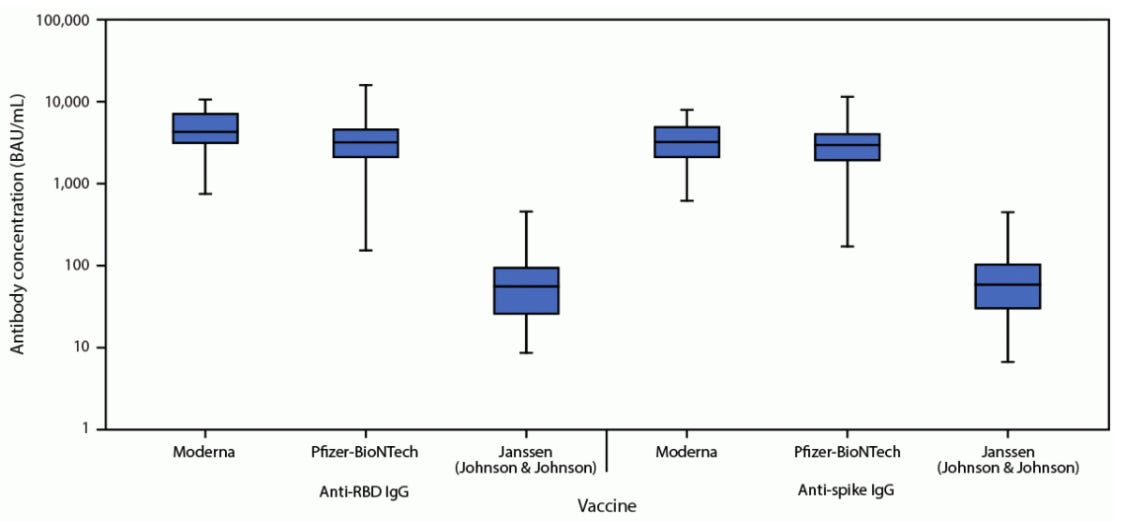
In the United States, we got a great look on Friday (September 17). The CDC published a study that assessed vaccine effectiveness across all three vaccines. They analyzed data from 3,689 hospitalized adults at 21 hospitals across 18 states during March-August 2021. Immunocompromised patients were excluded. What did they find?
J&J effectiveness against hospitalization was 71% (Moderna was 93% and Pfizer was 88%)
Over time, there was a small decrease in protection against hospitalization (68% vaccine effectiveness). But the math told us that this wasn’t different than 71%.
J&J folks also had significantly lower number of antibody levels compared to mRNA folks. Unfortunately, we don’t know what a “good” antibody level is; we just know that sometimes lower numbers means not as protected.
Unfortunately, the number of J&J people in this study is very small (only 113 hospitalizations). So, we couldn’t accurately examine how vaccine effectiveness differed across risk factors (like age, comorbidities, etc.).
Booster Effectiveness
So, naturally the next question is… does an addition shot help?
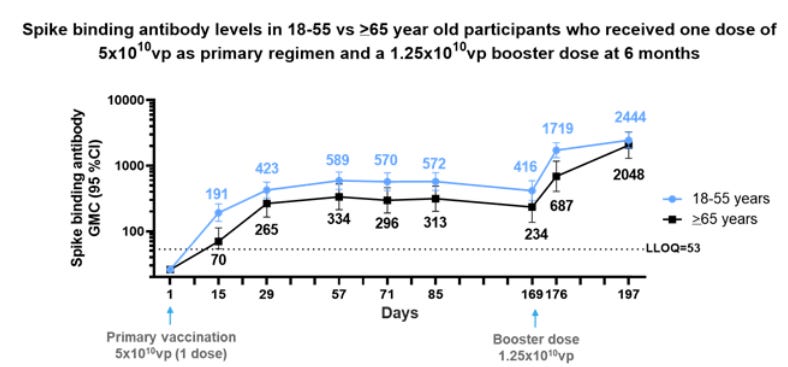
On August 25, J&J announced a preprint study. They conducted a randomized control trial of people previously vaccinated with its single-shot vaccine. Scientists wanted to answer three questions:
Does a second shot (same regimen as first shot) help increase antibodies?
Does a booster shot (smaller regimen that first shot) help increase antibodies)?
Does this differ by age (<65 years vs. 65 years older)?
They found…
Those with the second J&J shot (same regimen) had a 9-fold higher number of neutralizing antibodies than those without the second shot
Those with the booster J&J shot (smaller regimen) had a 6-7.7 fold higher number of neutralizing antibodies than those without the second shot
The increase in antibodies didn’t change based on age

Mixing Shots
There are zero, published or unpublished, data on the safety or effectiveness of mixing a J&J shot with an mRNA shot or series.
However, there is data on mixing AstraZeneca with Pfizer in the UK. This could be useful because the AstraZeneca shot is the same biotechnology as J&J. In other words, they are designed to do the same thing in the body. We can look at this data to make (very careful) inferences.
Mixing AstraZeneca with Pfizer is safe. There was one disadvantage though: you will get more side effects (e.g., headache, fatigue). But this is short lived. This data was published in a Lancet study (I previously posted about this study in detail here).
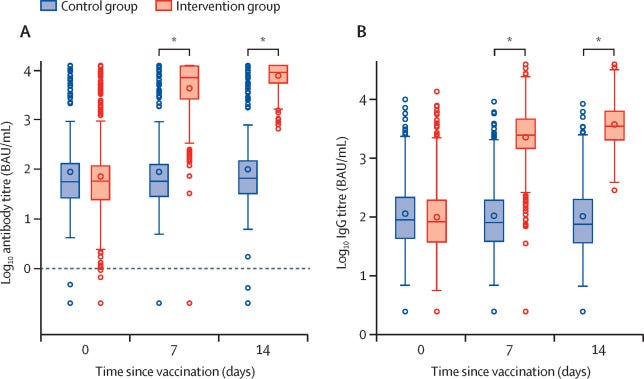
Mixing AstraZeneca with Pfizer is also highly effective. Another study published in Lancet found that it’s much more effective compared to just two shots of AstraZeneca or two shots of Pfizer.
We hypothesize this is because we’re mixing biotechnologies. We’re equipping our body to recognize the virus in different ways.
What should I do?
I was going to end the post there. But I know that I’ll get thousands of messages asking for guidance: What should I do? I can’t answer this for you. We have very little data on a second J&J dose. We don’t have any data on the safety or effectiveness of mixing J&J with an mRNA vaccine. There is some risk to going off label. And everyone has a different risk tolerance.
We will eventually get a solid answer to this question. I know a lot of studies are being conducted right now. But this takes time. And I recognize that J&J people, especially high risk (65+ years, those with comorbidities, and those in high risk occupations), want to protect themselves now. And sometimes we have to make decisions based on limited data.
I can answer this question for myself. If I got the J&J vaccine, I would check-in with my clinician to discuss my risks of COVID19 and the benefits of a second dose. But, it’s important to note that clinicians can’t formally advise either. A second dose for J&J is not approved by the FDA. After having this discussion with my clinician, I would go get an mRNA vaccine. I wouldn’t have done this before, but I’m not liking these recent J&J hospitalization effectiveness numbers from the CDC.
Someone I greatly admire, Dr. Angie Rasmussen, a brilliant virologist, got the J&J shot first and then decided, back in June, to get an mRNA dose. You can read her thought process on Twitter here, where she talks about weighing risks with benefits.
Bottom Line: We don’t have much data and it’s more than frustrating. The J&J vaccine isn’t as effective against hospitalization as Moderna or Pfizer. But there is still some protection. Some small studies have shown that getting a second J&J dose increases antibodies. There is no data on mixing J&J with mRNA vaccines, so there is risk by going off label. I and Dr. Rasmussen would take that risk, but that doesn’t everyone would.
I hope this helps you make a data-informed decision,
YLE





I am in the J&J Phase Three 1-shot Ensemble trial.
I received my vaccination in late November 2020. I did NOT get the placebo: got the real thing
I am at 10 months past vaccination.
.Thank you for this info as it is helpful as most who were not in the placebo group received our J&J vaccinations a lot earlier than the general community: I think from October to December 2020.
This is such a great synopsis. I'm wondering what effect the JJ news of this morning re. 2 and 6 month responses to an additional dose of the JJ vaccine has on your thinking? I've been considering seeking an additional MRNA shot, and this post convinced me that it is the right decision for me. Then, of course, this morning's announcement came out, and I am second-guessing again. I'm wondering if you have looked at the JJ extra dose data and have any perspective on whether that information changes your (hypothetical) calculus about whether combining vaccine types vs. sticking with JJ seems likelier to elicit a better and potentially more durable response?