The CDC published a study last week breaking down the numbers among pregnant people. Scientists used data from the Vaccine Safety Datalink (VSD) database, which is basically a network of hospitals in 8 states (CA, OR, WA, CO, GA, MN, WI, and MA).
From December 14 to May 8, 135,968 pregnant people were seen at the VSD hospitals. Among these people, only 16.3% had received at least one dose of the vaccine; 11.1% were full vaccinated.
Notice that the 8 states participating in VSD are also some of the highest vaccinated states overall. So, 16.3% is likely an overestimate of the “true” rate of vaccinated pregnant people in the United States. Which is, obviously, not good.
Who is the least likely to be vaccinated?
Pregnant people aged 18-24 years, as only 5.5% received a vaccine (compared to 16.2% among those aged 25-34 and 22.7% among those aged 35+)
Non-Hispanic Black pregnant people (only 6% were vaccinated) and Hispanic pregnant people (only 11.9% were vaccinated; compared to 24.7% of Asians and 19.7% of Whites)

Why do we care?
Pregnant people (and unborn babies) are at higher risk for severe COVID-19 disease. By now this is well-established, as there have been 42+ studies on this topic thus far. Pregnant people with COVID-19 disease are…
…more likely to go to the ICU, need ventilation, and/or need oxygen compared to non-pregnant (here)
…more likely to have preeclampsia (here)
…more likely to have babies born preterm (here) or stillborn (here)
…more likely to have their babies admitted to the neonatal unit (here)
And we know vaccines are safe during pregnancy.
Pregnant people were deliberately excluded in the first round of COVID19 vaccine clinical trials. This is normal practice. However, as of June 14, 124,597 pregnant people had received the vaccine. The CDC is currently following 5,102 of them. (If you’re pregnant, vaccinated, and want to participate in the ongoing study go HERE). Last week, the New England Journal of Medicine published, for the first time, some results of this CDC cohort.
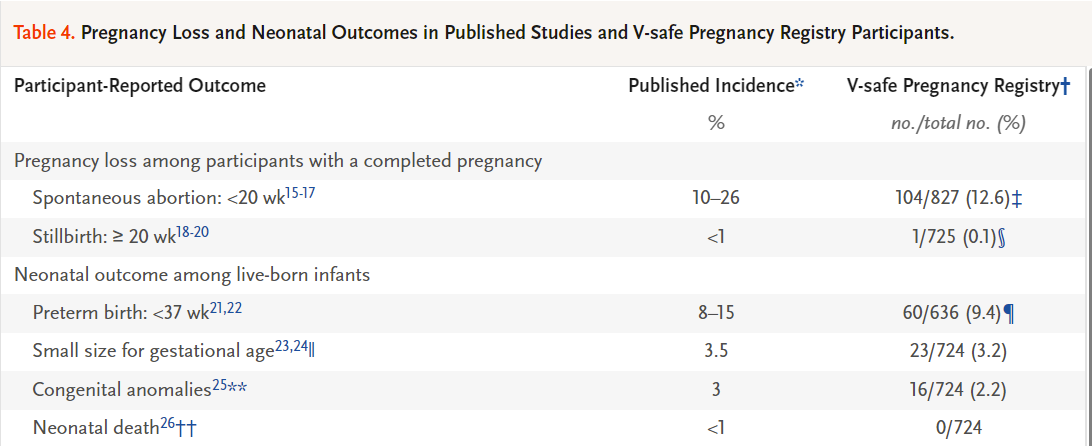
What did they find? No unexpected pregnancy or infant outcomes have been observed related to COVID-19 vaccination during pregnancy. Specifically, among the 3,958 participants, they found:
28% received their vaccine in the 1st trimester, 42% in the 2nd, and 26% in the 3rd
0.3% breakthrough infections occurred (or 12 people got COVID19 after being fully vaccinated; this is about the same rate as in the general population)
827 completed pregnancy:
712 (86.1%) resulted in a live birth
115 (13.9%) resulted in a pregnancy loss
Pregnancy loss, preterm birth, babies size, congenital problems, and death was not different among those with the vaccine compared to the background rate.
Vaccines protect the babies (once they’re born) too!
If a pregnant person gets vaccinated, there is mounting scientific evidence showing that babies get protection too. Both through antibodies crossing the placenta (here, here, here, here, here, here, here) and breastmilk (here, here, here).
I had a baby in October 2020 and am still very bummed I couldn’t get vaccinated while I was pregnant. If I did, she would have had some sort of protection right now (instead of having to wait until 2022 for the vaccine).
And, yes, you still need the vaccine even if you’ve already recovered from COVID-19 (before or during pregnancy).
There are four main reasons, which you can read more about here. The same reasons apply for pregnant people.
Bottom Line:
If you’re pregnant, get the vaccine. It’s good for you. And, if that’s not a good enough reason, it’s good for the baby.
We (as clinicians and public health officials and journalists and family members and neighbors) need to improve outreach and engagement with pregnant people. We need to get this vaccine rate up fast! And we all have a role to play.
Here is a 1-pager I threw together that can help guide you through the tough conversations. As always, if you’re a paying subscriber, reply to this email and I can send you a PDF.
Love, YLE





I have a Hispanic (Mexican) grandma who is hesitant (lives in Austin, TX). From what I understand her fear is that vaccines are causing deaths, among other disinformation. I think she gets a good deal of this disinformation from Mexican news sources and (some of my) family, which I am less equipped to understand. I’m going to make my case for her to get the vaccines as she is actually very high risk (beyond just old age). Can someone advise how I could approach this for someone who is semi-“foreign”?
Any idea when we’ll finally get information about the safety of the vaccines while breastfeeding? I keep checking. The cdc website still says this:
“Clinical trials for the COVID-19 vaccines currently authorized for use under an Emergency Use Authorization in the United States did not include people who are breastfeeding. Because the vaccines have not been studied on lactating people, there are no data available on the:
Safety of COVID-19 vaccines in lactating people
Effects of vaccination on the breastfed baby
Effects on milk production or excretion“