Si quiere leer la versión en español, pulse aquí.
One thing is consistent after the peak of every wave: A highly charged debate on how we move forward as individuals, as a community, as a nation, and as a globe. For example, right now we have one side suggesting to drop masks from here on out and another side that says keep mask mandates.
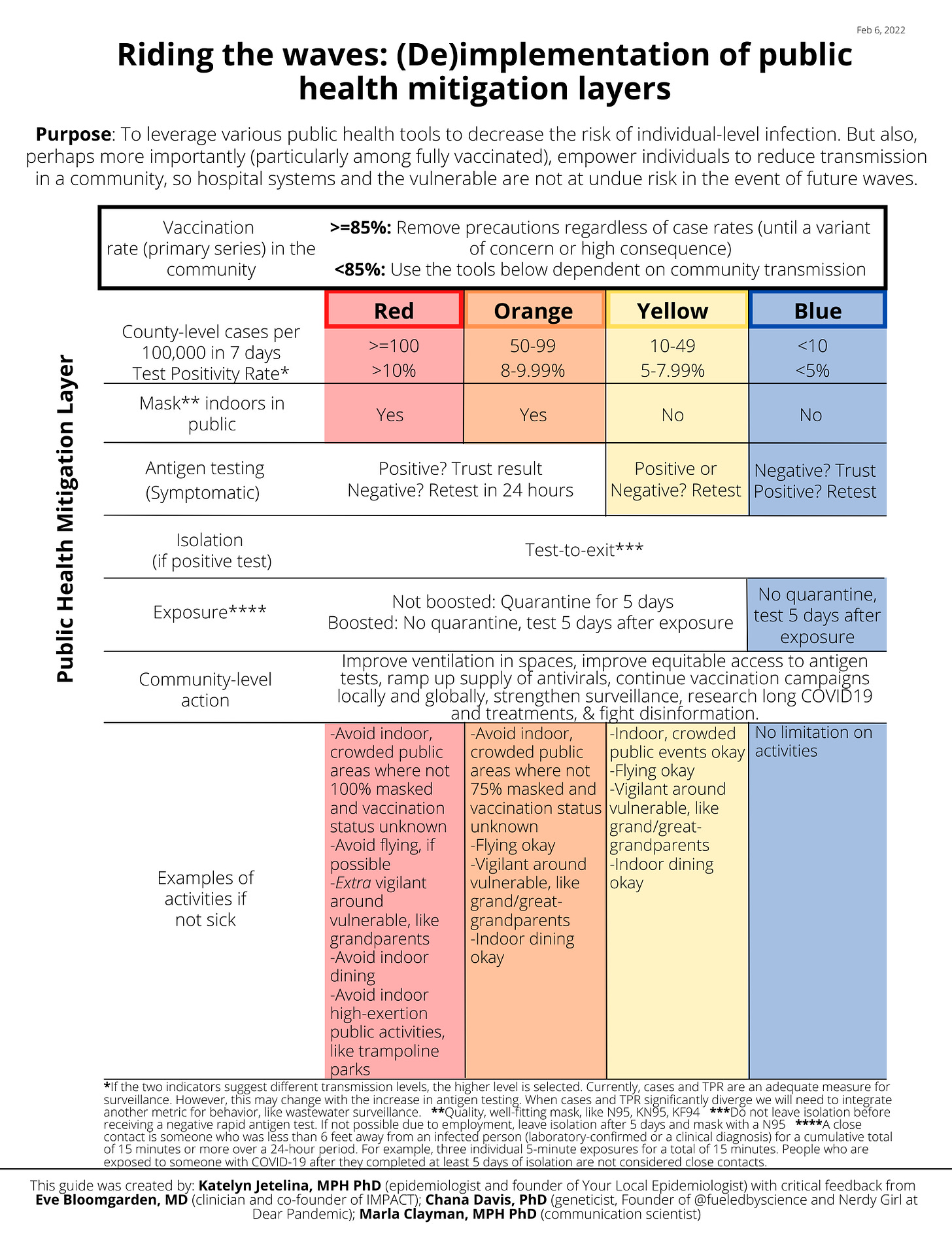
I find both sides problematic, because reality is not binary and the future is unknown. We need a solution that addresses the ebb and flow of viral dynamics. I strongly believe we do this by riding the waves and leveraging the tools we have at hand. This will protect individuals and populations when transmission is high and ensure a much needed break with transmission is low. I worked on a framework (for longer than I want to admit) to reflect this line of thinking. In constructive, critical, and lengthy discussions with colleagues, this is what we came to:
There are a few things in this framework to call out:
Individual-level: This is for individual decision making. In other words, it answers: What should I do today? As a public health official, I do not agree that we need individual-level solutions. They are far less effective than population-level ones. But in our increasingly individualistic society, we need to arm people with evidence-based solutions in the landscape they are forced to navigate.
Use of cases. This framework is anchored by cases. Much to my surprise, COVID-19 metrics largely held up during the Omicron wave: test positivity rate was followed by case trends, which was followed by hospitalizations and deaths. I suspect this will change with time. When cases and TPR diverge, we’ll need to integrate another metric for behavior, like wastewater surveillance. Some scientists propose to use hospitalizations and deaths metrics to drive decision-making, but I strongly disagree because once these metrics start increasing, it’s too late—transmission is already been at uncontrollable levels for 3-4 weeks prior.
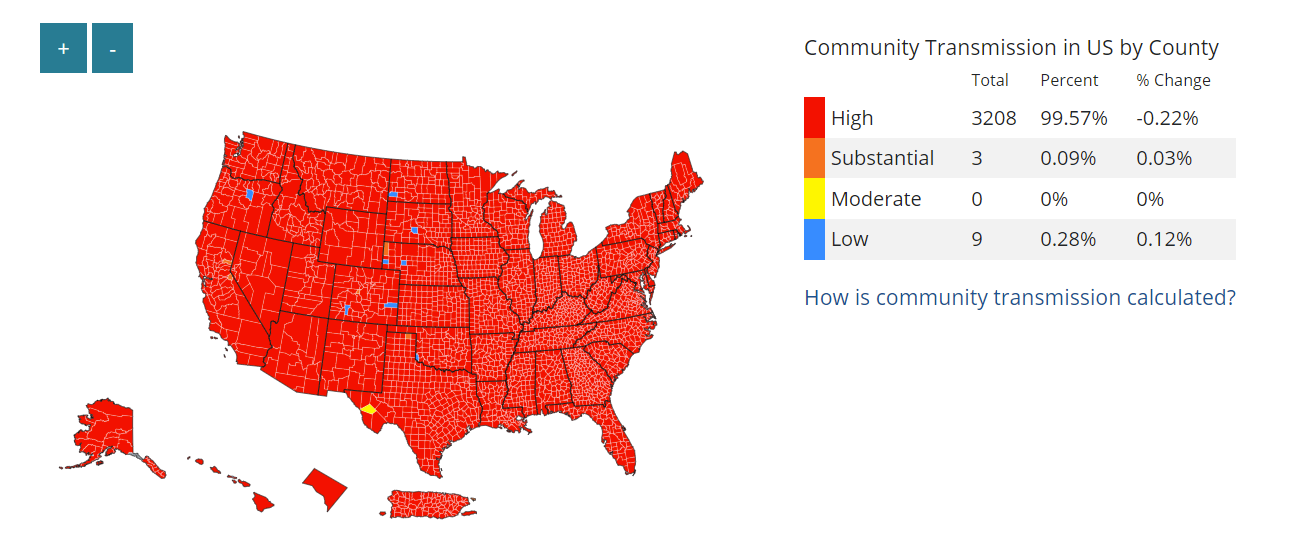
In addition, leveraging cases/TPR surveillance improves feasibility, because the CDC provides this metric for every county in the U.S. here. (For the record, 99% of counties are still in the red right now.)
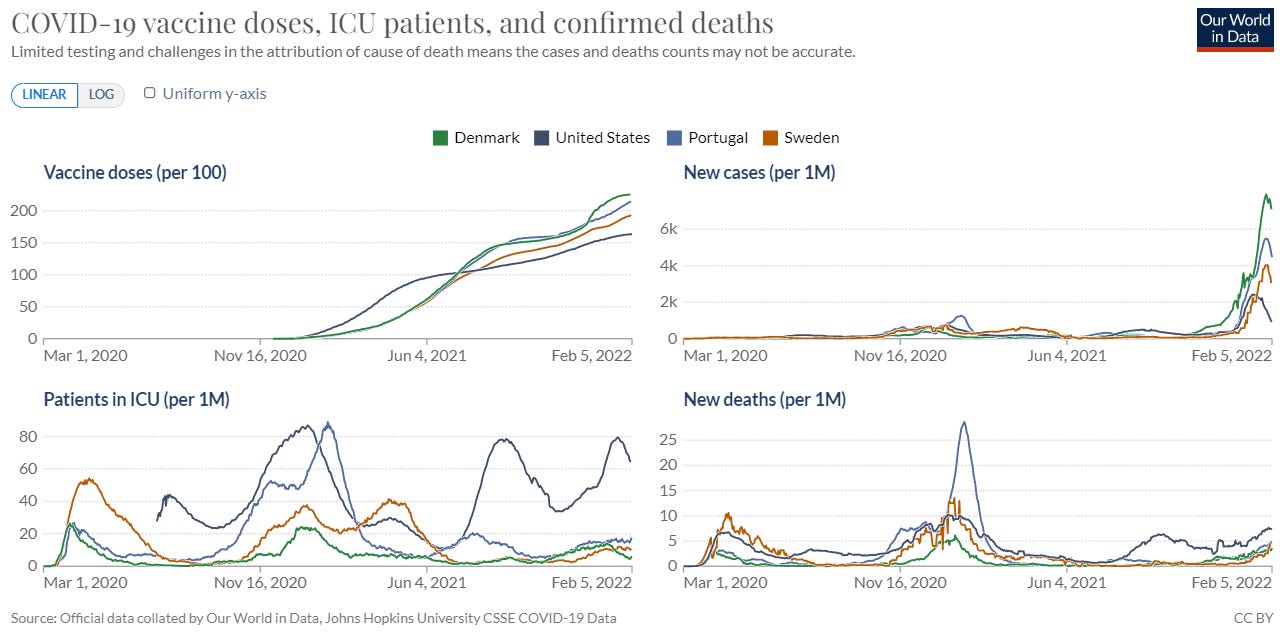
Vaccination rate of 85% of total population. I deliberately included a vaccination cut-off point at 85% to indicate removing precautions regardless of case rates. Several countries, like Denmark and Sweden, are lifting all restrictions. And, I support this because their vaccination rates are high. During the Omicron wave, it was blaringly obvious that this high vaccination rate reduced burden on their healthcare systems. Below are four graphs with key COVID19 metrics across Denmark, Sweden, Portugal, and the U.S. The U.S. has, by far, the lowest rate of vaccine doses per person. The U.S. also had overwhelmed hospitals with record breaking ICU numbers and deaths (this metric is still increasing, so this may eventually break records, too). This did not happen in the other countries.
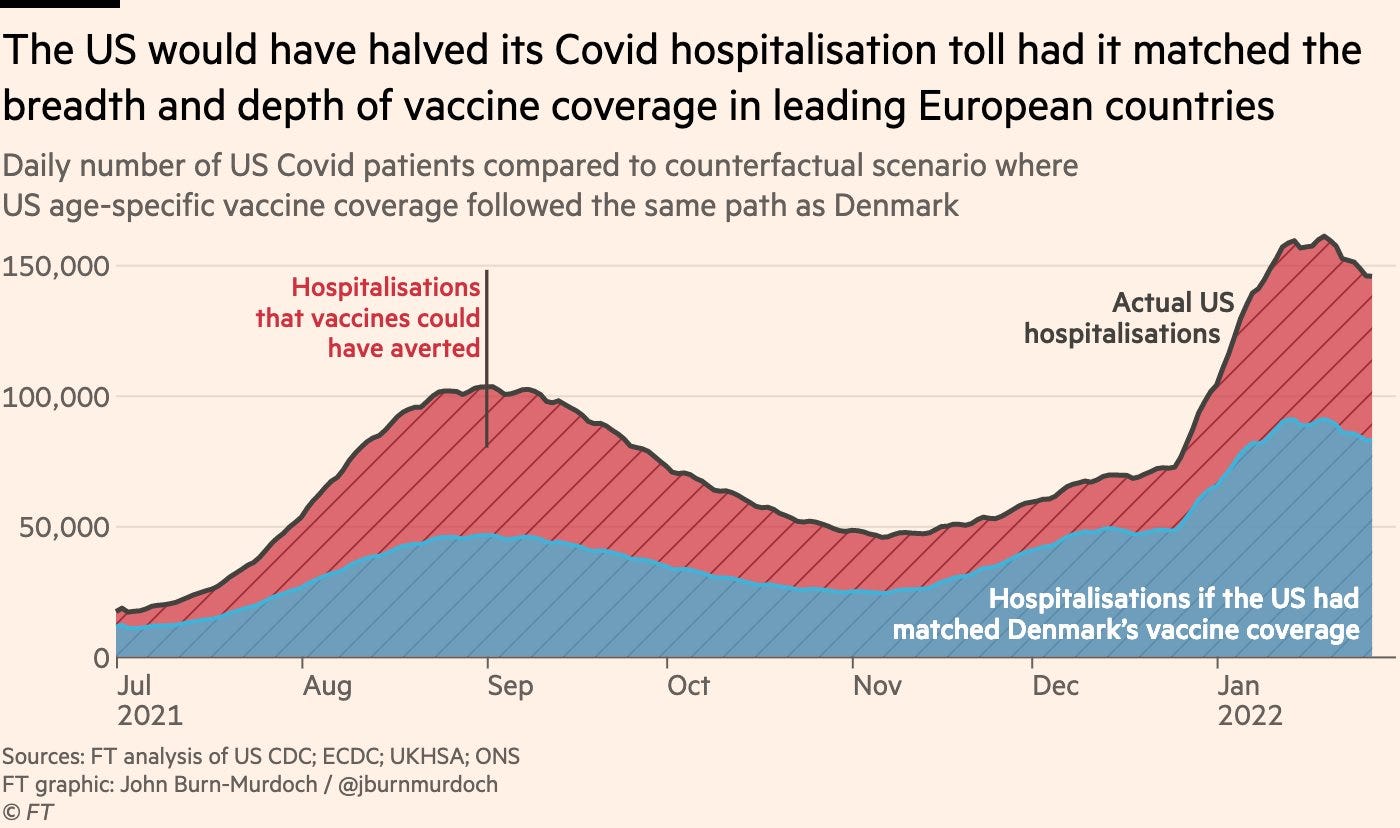
As John Burn-Murdoch from the Financial Times pointed out, if the U.S. had the same breadth and depth of vaccination as Denmark, hospitalizations would have halved during this recent wave.
Community-level action. Even though Denmark, for example, has a high vaccination rate, they still had very high community transmission of Omicron. So removing precautious with a >85% vaccination rate will not protect the vulnerable or address the global problem. This is why the “community-level action” line in the framework is critical.
Example of activities. This is highly dependent on risk tolerance. Throughout the pandemic, I’ve had a “moderate” risk tolerance, in part because my girls are ineligible for vaccines. But even when my girls are fully vaccinated, I will continue to follow this framework. Not because I’m worried about our individual-level risk (vaccines work amazingly!), but because of the very real population-level risk with high transmission and low vaccination rates.
Bottom line: We need a framework that accounts for an uncertain future. Maybe this was our last wave, and we’ll either reach 85% vaccination rate or be in the “blue” for the foreseeable future. But in the likelihood that this isn’t the last wave, we can prepare and leverage effective tools to reduce individual-level and population-level risk. My family and I will be riding the waves. I invite you to join us.
Love, YLE
Here is the PDF download (English and Spanish) for paying subscribers. Put it on your refrigerator, share with others, or use it as doodling paper: