Si quiere leer la versión en español, pulse aquí.
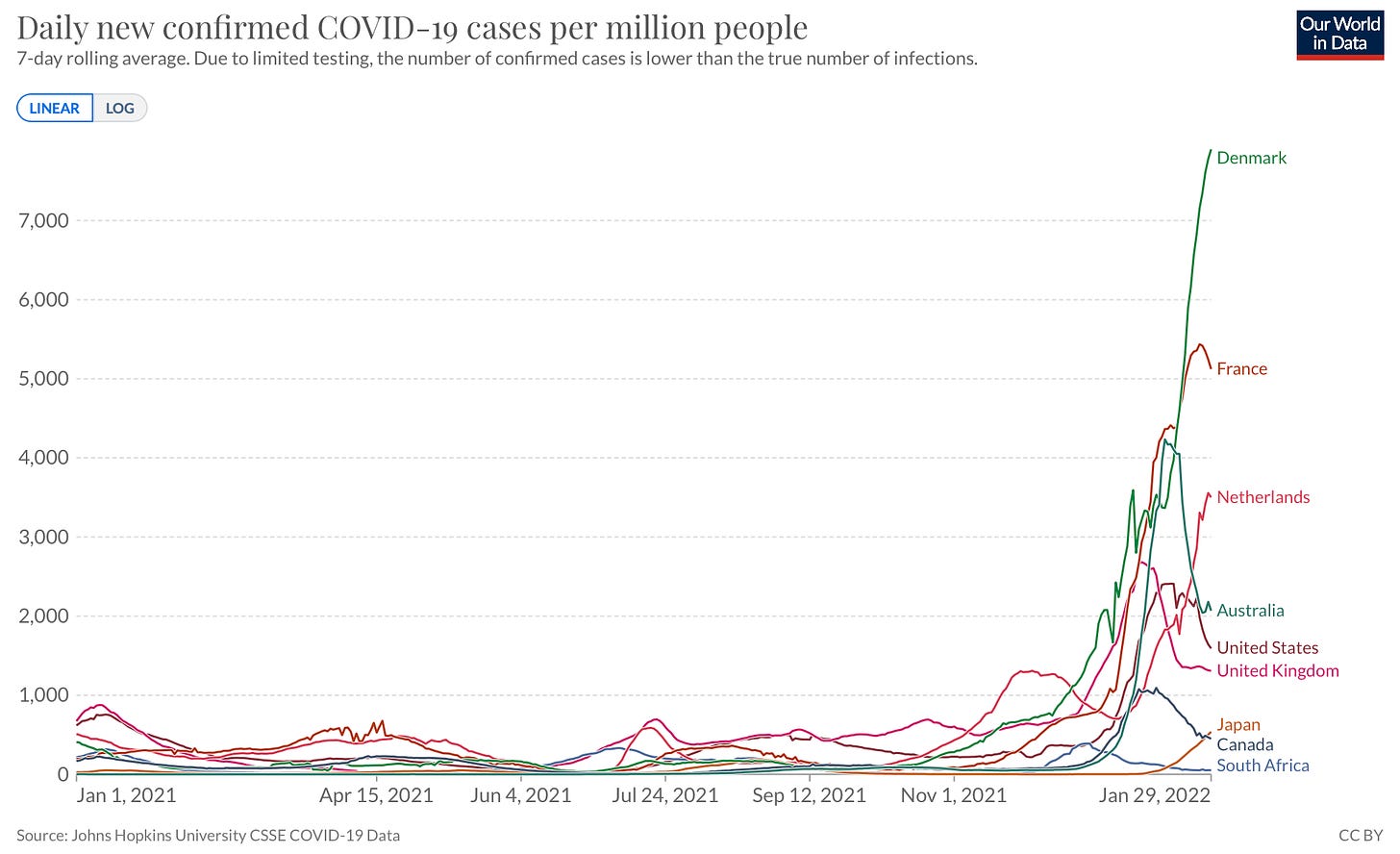
Well, case patterns continue to vary greatly across the world. For example, after reaching ridiculous heights, France and Australia are on the descent. Japan’s cases are gaining speed, and interestingly, U.K., Canada, and South Africa have stalled after their initial descent.
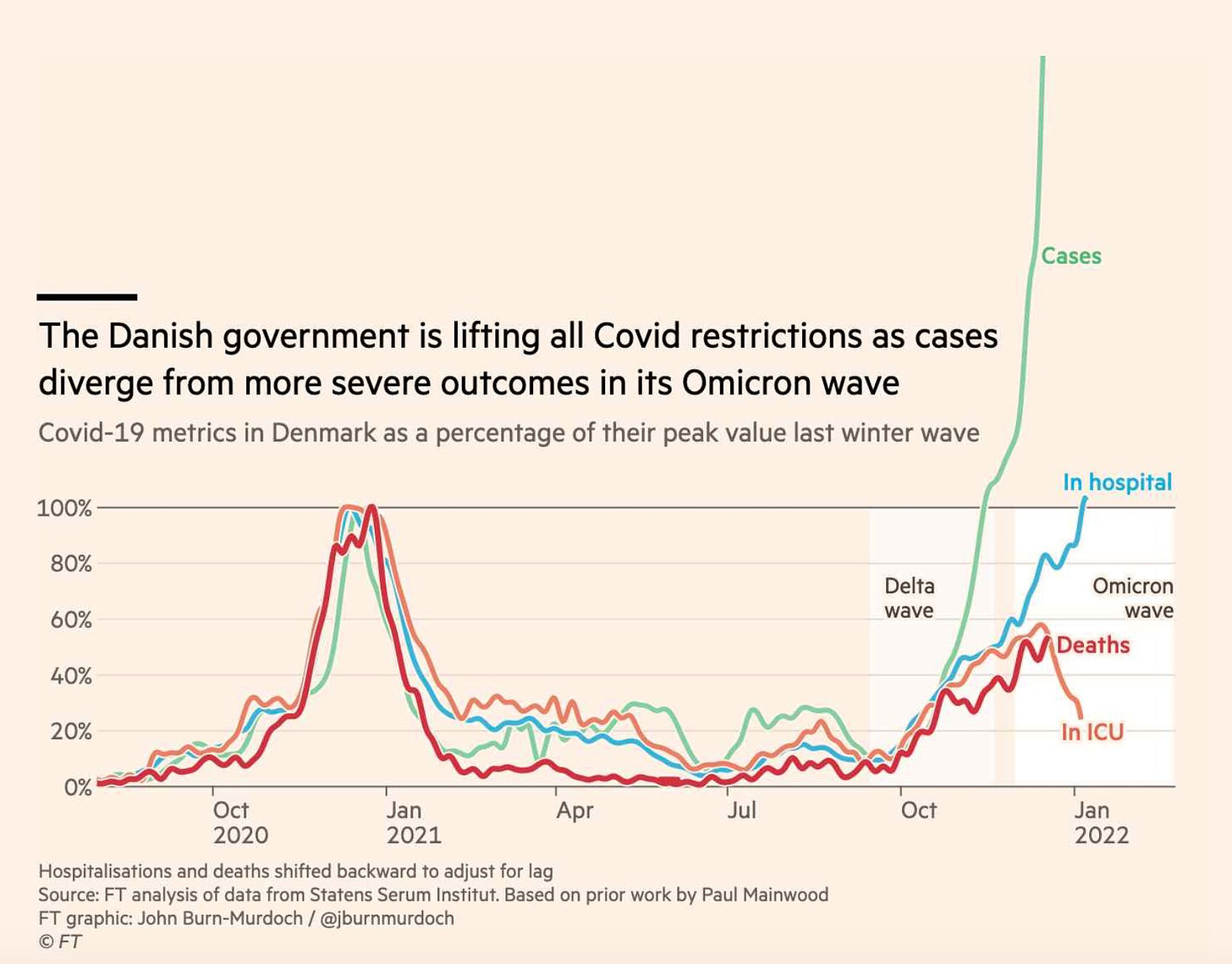
Denmark’s out-of-this world cases continue to increase. I thought this dramatic figure from John Burn-Murdoch at Financial Times was spot on; it also highlights that ICU rates are decreasing and deaths are about 50% of that of their last winter wave. With an 83% vaccination rate, Denmark decided to remove all COVID19 public health mitigation measures—which, as you can imagine, has caused quite the international debate.
BA.2 Update
The mix of case patterns across the world is likely attributed to BA.2 (the sister lineage of Omicron) taking hold. The WHO confirmed that investigating BA.2’s ability to induce severe disease and to escape prior immunity should be prioritized. Since my update last week, we’ve learned a little more about this sub-lineage:
Transmissibility. We have consistent evidence that BA.2 outcompetes BA.1. In England, for example, BA.2 has a +126% growth rate over BA.1. Secondary attack rates in U.K. households are also higher: 13.4% of BA.2 cases transmitted within their households vs 10.3% of BA.1. The graph below, which displays the variant growth in Denmark, confirms a growth advantage. Importantly, as seen in a study of Denmark households, vaccination helped protect against transmission more for BA.2 than BA.1.

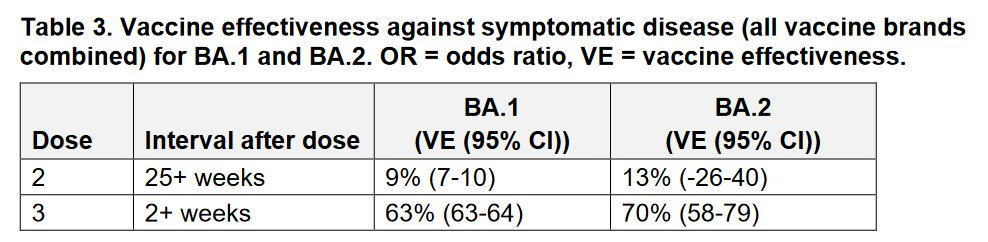
(Chart from Pandemic Prevention Institute Here) Immunity escape. We have preliminary evidence that vaccines continue to work great against BA.2. In fact, they work a little better than against BA.1. The U.K. Health Security Agency released a report last Friday suggesting vaccine effectiveness against symptomatic disease was 70% for BA.2 compared to 63% for BA.1. This is great news.
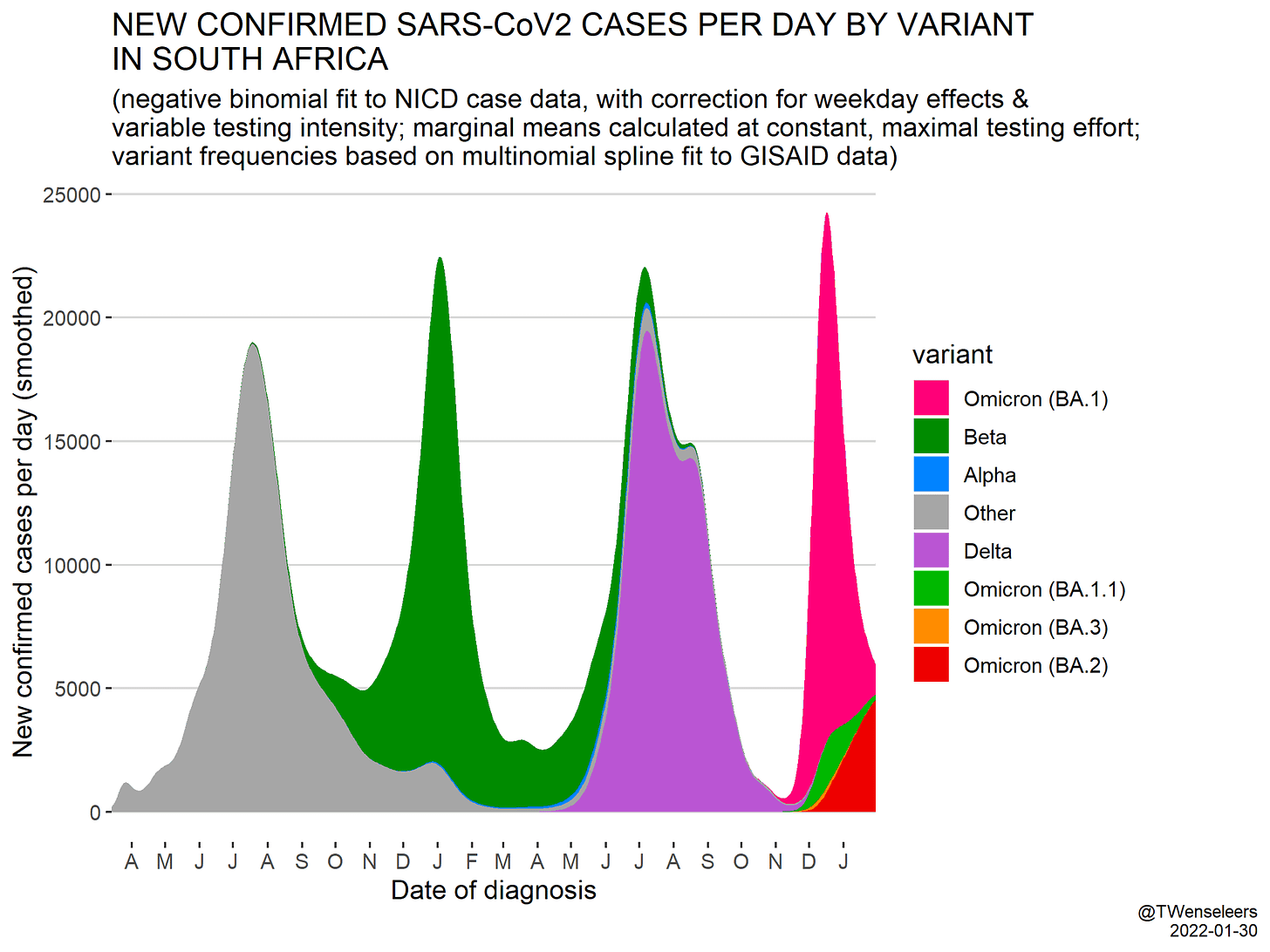
So, BA.2 means that we’ll likely see a prolonged Omicron wave across many countries. For example, in South Africa cases are due to start increasing because BA.2 is taking hold. How much cases increases, though, will be important to closely follow over the next few weeks.
United States
In the United States, cases and test positivity rates continue to decline. Because both metrics are mirroring each other (rather than showing opposite trends), I’m confident this is the “true” trend and not a testing capacity or testing behavior phenomenon. The raw number of cases, though, continues to be greatly underreported. Because of the massive blizzard in the Northeast, numbers may be off this upcoming week due to delayed testing, closed labs, and people staying home.
The case trend seems to be consistent across all U.S. regions. In fact, there are only 10 states with case growth right now, with Montana (+79%), Washington (+55%), and Idaho (+46%) as the leaders. But even the leaders have less than impressive growth compared to at the beginning of the Omicron wave when we were reaching 4-digit percentage increases.
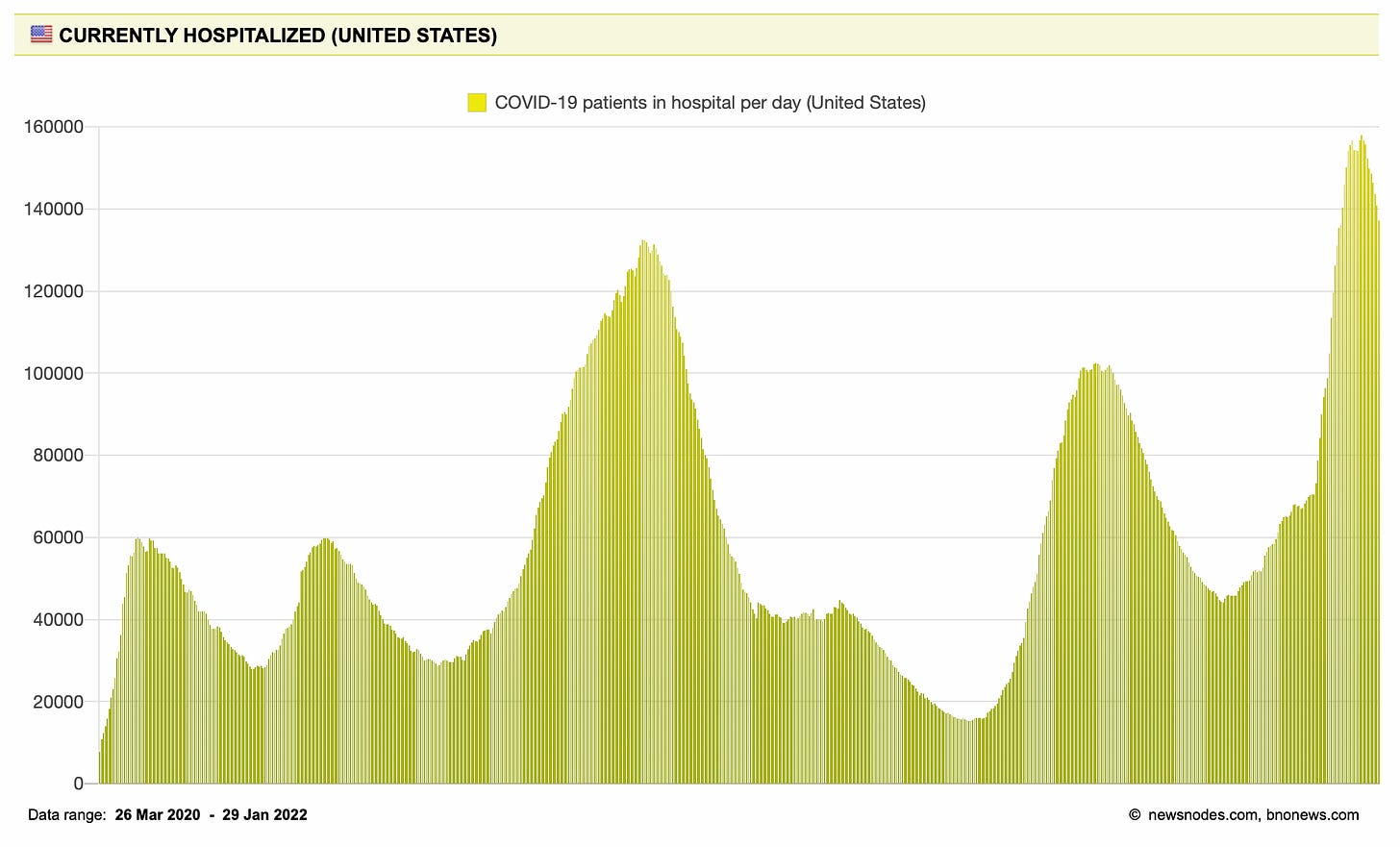
Unfortunately, hospitalizations and deaths continue to lag cases. And while hospitalizations continue to decline, they are still very high at 146,787 people hospitalized. This means we are still above last winter’s hospitalization peak. Deaths haven’t peaked yet and have increased 29% in the past 14 days. Last Friday, we recorded 3,824 deaths in. one. day. On average, we are losing 2,572 people per day.
Thanks to immunity, treatment, and an intrinsically less severe Omicron, the case fatality rate (CFR) continues to decline in the Untied States and across the globe. We’re seeing a similar pattern in infection fatality rate (IFR— which takes into account asymptomatic and non-reporting) in the U.K. But, as seen in the second graph below, IFR is still about two times higher than the flu. (Keep in mind this means U.S.’s IFR is about two times higher than the U.K.’s). Even though COVID19 is getting less and less lethal on an individual-level, COVID19 is also getting more and more transmissible. In places like the U.S. with suboptimal vaccination breadth and depth, the two are essentially cancelling each other out and COVID19 continues to make a big impact on population-level metrics, like death.
Vaccinations
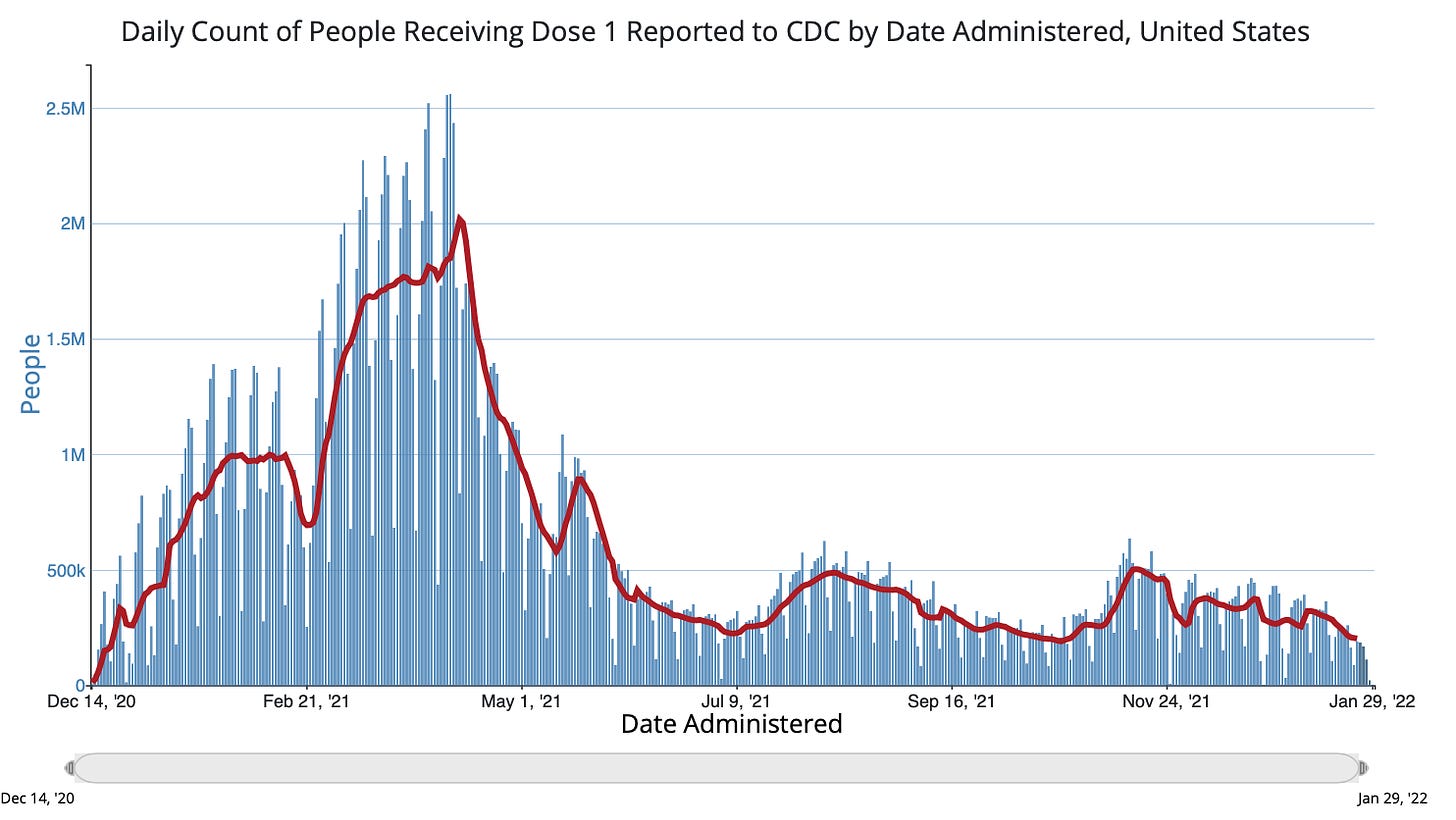
In the United States, 67.7% of people aged 5+ have the primary series (63.7% of the total population). And, as we’ve seen in previous waves, Omicron’s silver lining was that more people got their first dose. This uptick was modest; the Kaiser Family Foundation reported only 8% of unvaccinated adults said Omicron made them more likely to get vaccinated. We are inching closer and closer to vaccination saturation. Yet vaccination rates continue to be disproportionately spread across a variety of sociodemographic groups.
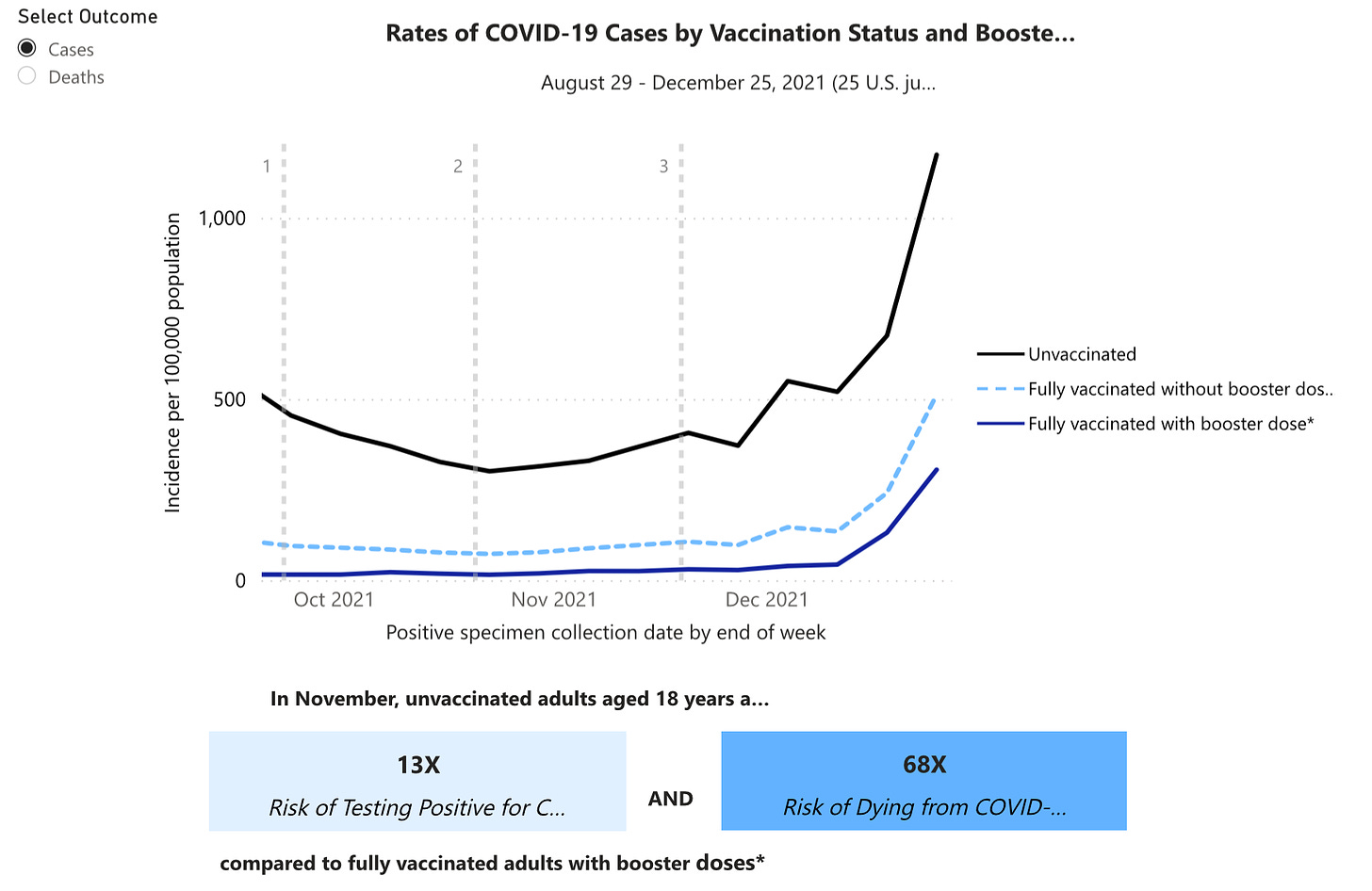
Among those who are vaccinated, only 41.3% are boosted. Even more worrisome to me is that only 64% of Americans 65+ years have a booster, as they are more likely to have severe breakthrough cases than younger populations. The number one reason people aren’t boosted is because they “don’t need it/don’t feel at risk from COVID” followed by “ineligible (hasn’t been long enough since last shot)” and “don't think it will be effective.” But the story continues to be clear: Boosters do help against infection, hospitalization, and death. But certainly not as much as getting vaccinated in the first place.
Have a wonderful week! YLE
“Your Local Epidemiologist (YLE)” is written by Dr. Katelyn Jetelina, MPH PhD—an epidemiologist, biostatistician, professor, researcher, wife, and mom of two little girls. During the day she has a research lab and teaches graduate-level courses, but at night she writes this newsletter. Her main goal is to “translate” the ever-evolving public health science so that people will be well equipped to make evidence-based decisions. This newsletter is free thanks to the generous support of fellow YLE community members. To support the effort, please subscribe here:







Just wanted to let you know that I shared this information, particularly the info on the effectiveness of boosters against the new variants, with the woman who cleans our house (and does myriad other things beyond my capacity). It convinced her to go get her booster shot today. So THANKS
(I just want to take a quick moment to say how much I appreciate your efforts to make all this data and technical information accessible and understandable to a general audience. As someone who develops technical documentation for a living, I know how much work it takes to do that well. Thank you!)