It’s heeeere. The official start of the respiratory season kicked off last week.
Here is your first State of Affairs for this fall/winter.
Influenza-like illnesses
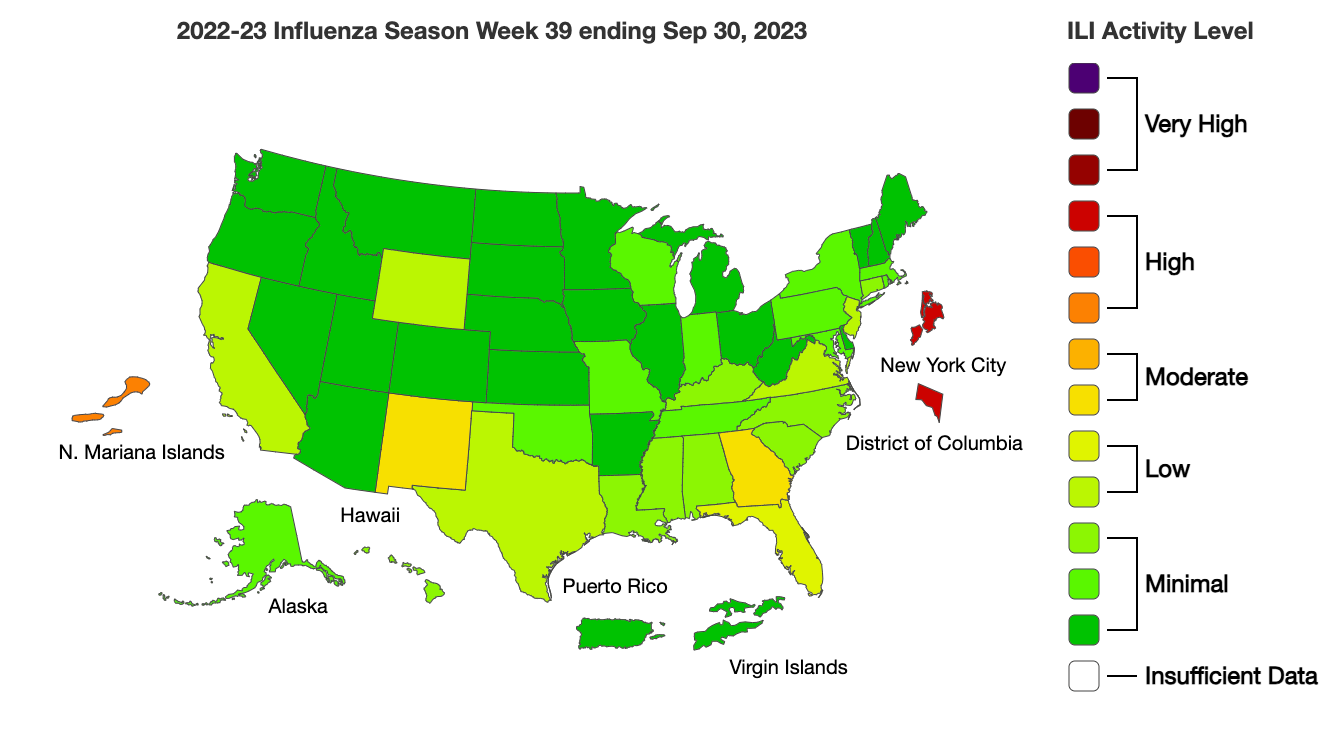
Every Friday, the CDC updates their “influenza-like illness” (ILI) data. This is a database where providers tally patients who presented with ILI—a fever, a cough, and/or sore throat—at their office. So these numbers include everything (flu, RSV, COVID-19, etc.) and are a general indication of the climate of respiratory health in the United States.
ILI is starting to creep up but is still below the “epidemic” level threshold. Last year we were hit early and hard. It will be incredibly interesting to see how this unfolds.

Low levels result in a pretty “green” picture of low activity across the United States. We will get to purple here in the next few weeks/months.
Here is a deeper dive into the “big three” viruses.
Covid-19: On the decline
After our summer wave, every Covid-19 metric is declining—wastewater, ED visits, and hospitalizations. This isn’t a surprise; we’ve consistently seen a lull in Covid-19 this time of year. We are exactly overlapping last year’s trends in wastewater.

Compared to the other big two (RSV and flu), Covid-19 hospitalizations continue to take the lead per capita.
However, there has been significant decoupling of hospitalization and case numbers due to population-level immunity. Although we continue to see waves of infection, COVID-19-associated hospitalizations remained consistently lower than in previous years. Progress.

Who is being hospitalized today? According to a new CDC report:
2 in 3 are adults over the age of 65 years
90% of those hospitalized had multiple comorbidities
3 in 4 hospitalized are not up-to-date on Covid-19 vaccine*
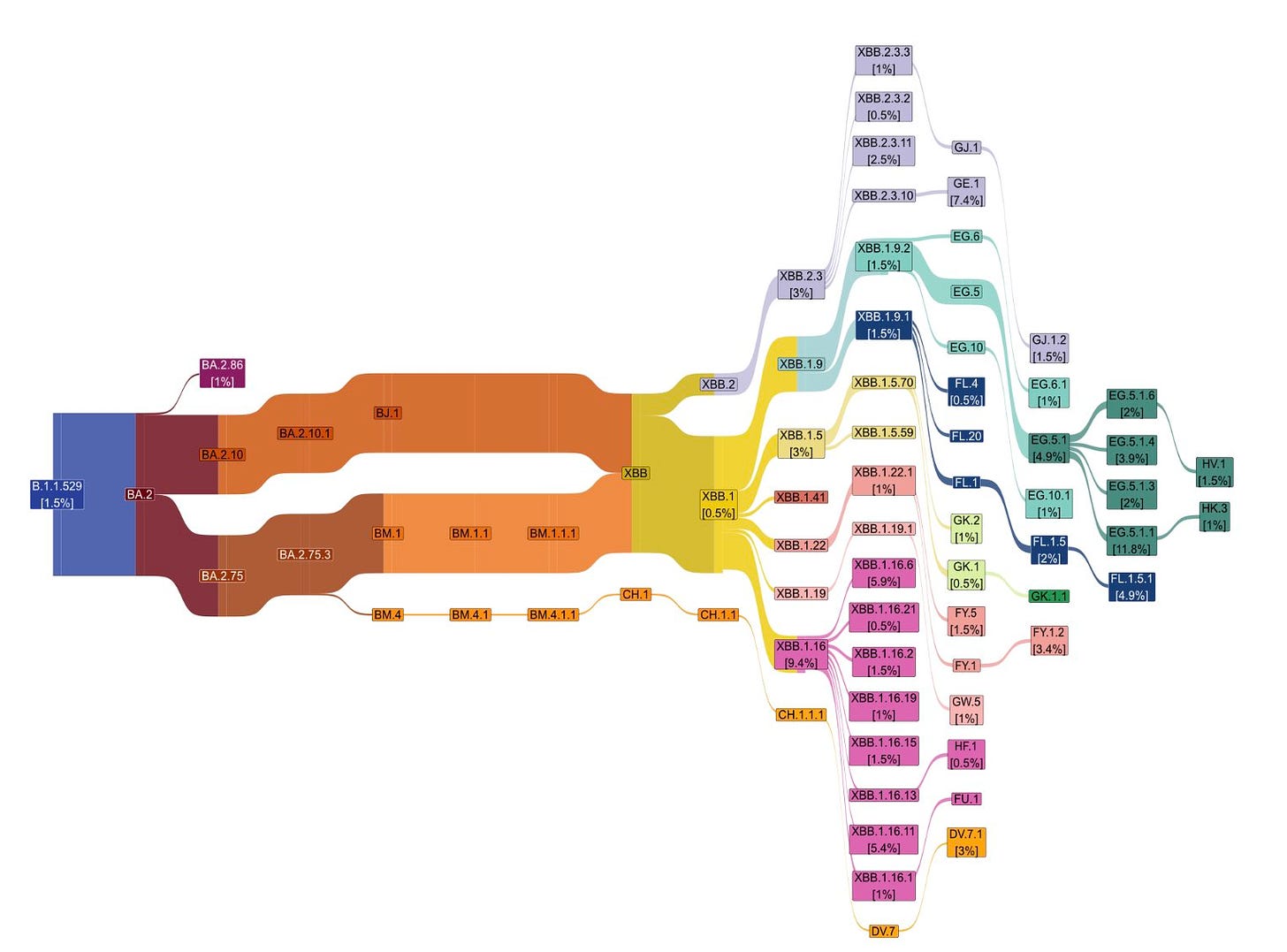
We are paying close attention to how Omicron continues to change. Below is a beautiful Sankey diagram showing the Omicron family tree. From left to right, it shows the 14 generations of Omicron over time, with the thickness of the line proportional to the number of sequences.
Two specific subvariants will likely drive our expected winter surge:
BA.2.86—the highly mutated variant we detected a few weeks ago—is sticking around. It’s now in 24 countries and showing a 30-45% growth advantage. This means it’s not fizzling out; it still has the potential for a wave but not a tsunami. It has already started to mutate, so it will be important to see what incremental changes it makes to increase its capability against our immunity.
FLiP mutations—a group of subvariants that have a combination of new mutations called FLip because they involve two L to F amino acid mutations—is gaining ground.
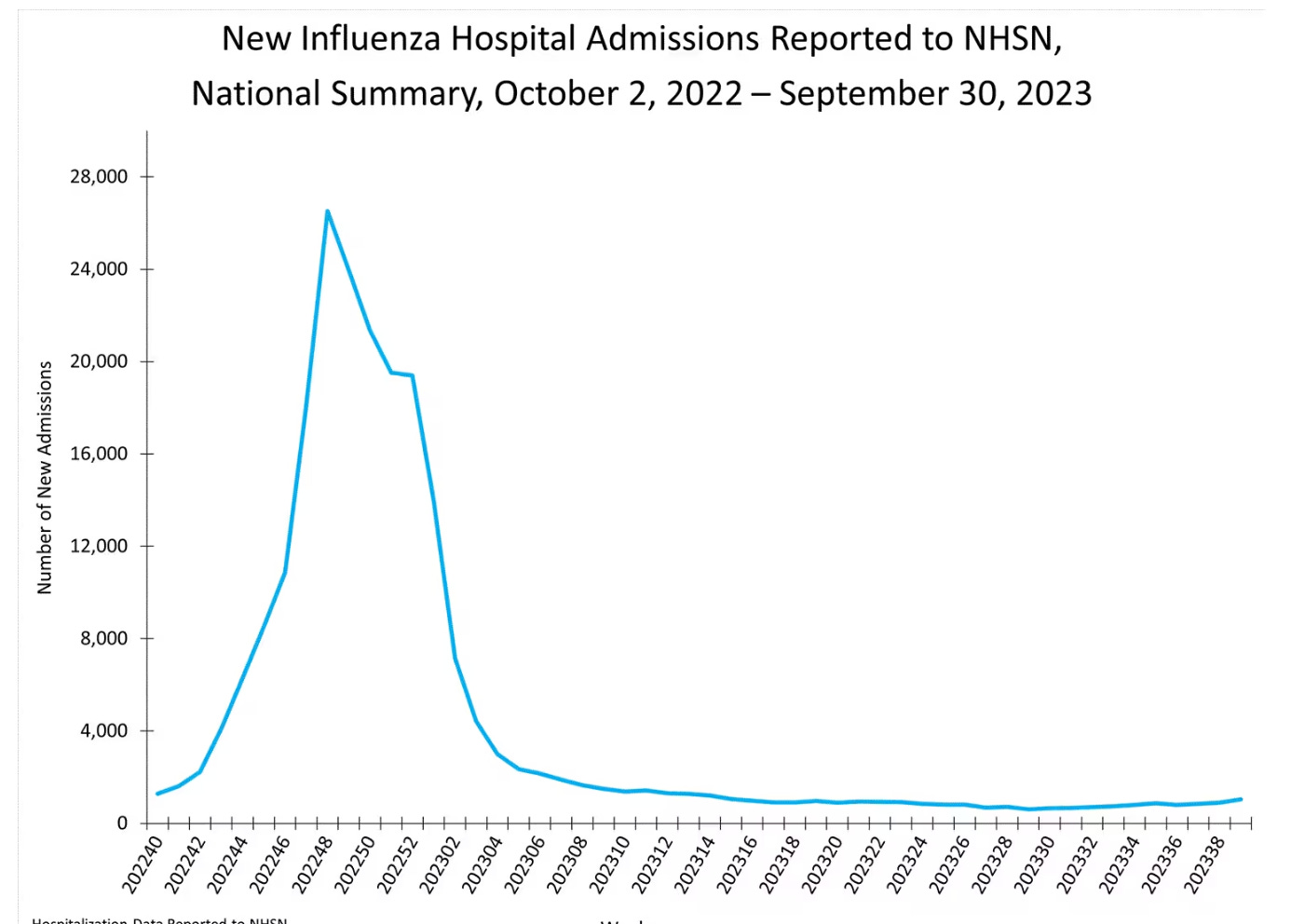
Flu: Very low levels
Influenza levels are still very low. Last week, 1,040 patients with laboratory-confirmed influenza were admitted to a hospital. This is compared to a typical peak of ~28,000.
Interestingly, one specific strain of flu—called Yamagata influenza B—has gone extinct due to Covid-19 measures. This is incredible news because of two things:
It wasn’t thought that we could eliminate a flu strain.
This strain was notoriously difficult to predict for flu vaccine strain-selection purposes. The WHO has officially recommended not including this strain in future vaccines.
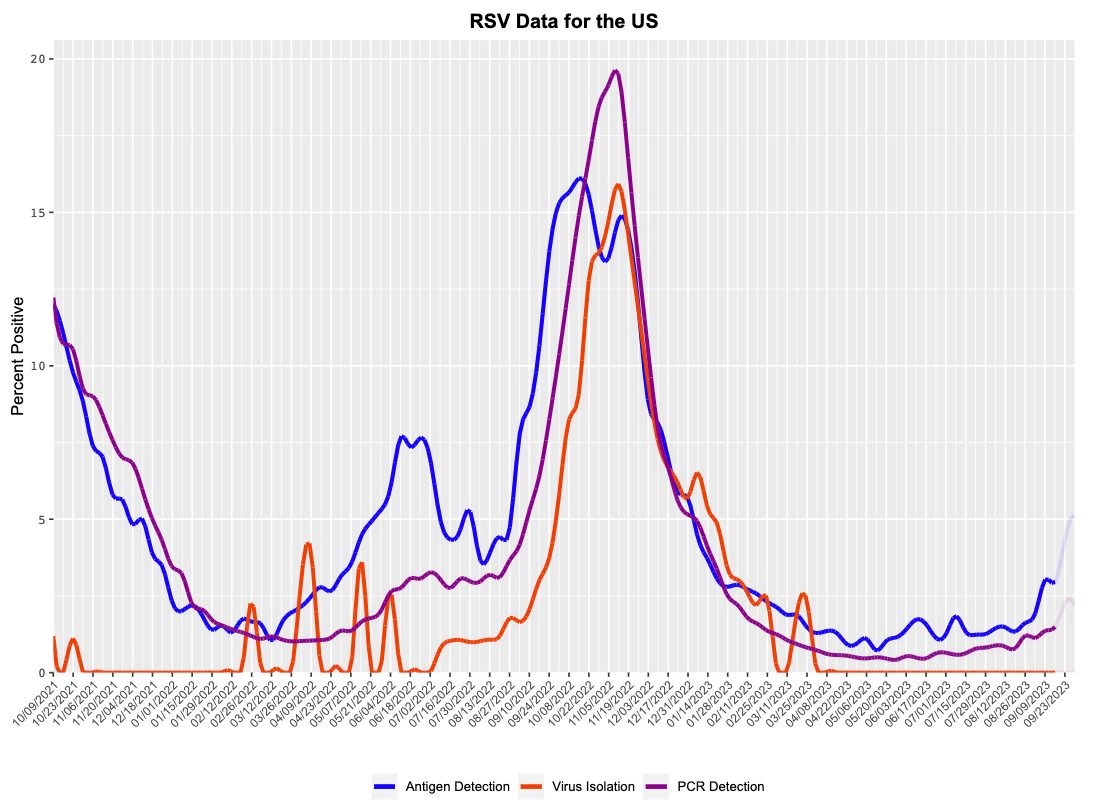
RSV: Heating up in the South
RSV is picking up. National trends are being driven by one region—the South. This typically signals the beginning of RSV season, in which the virus will subsequently spread to the Northeast and West over the next two months.
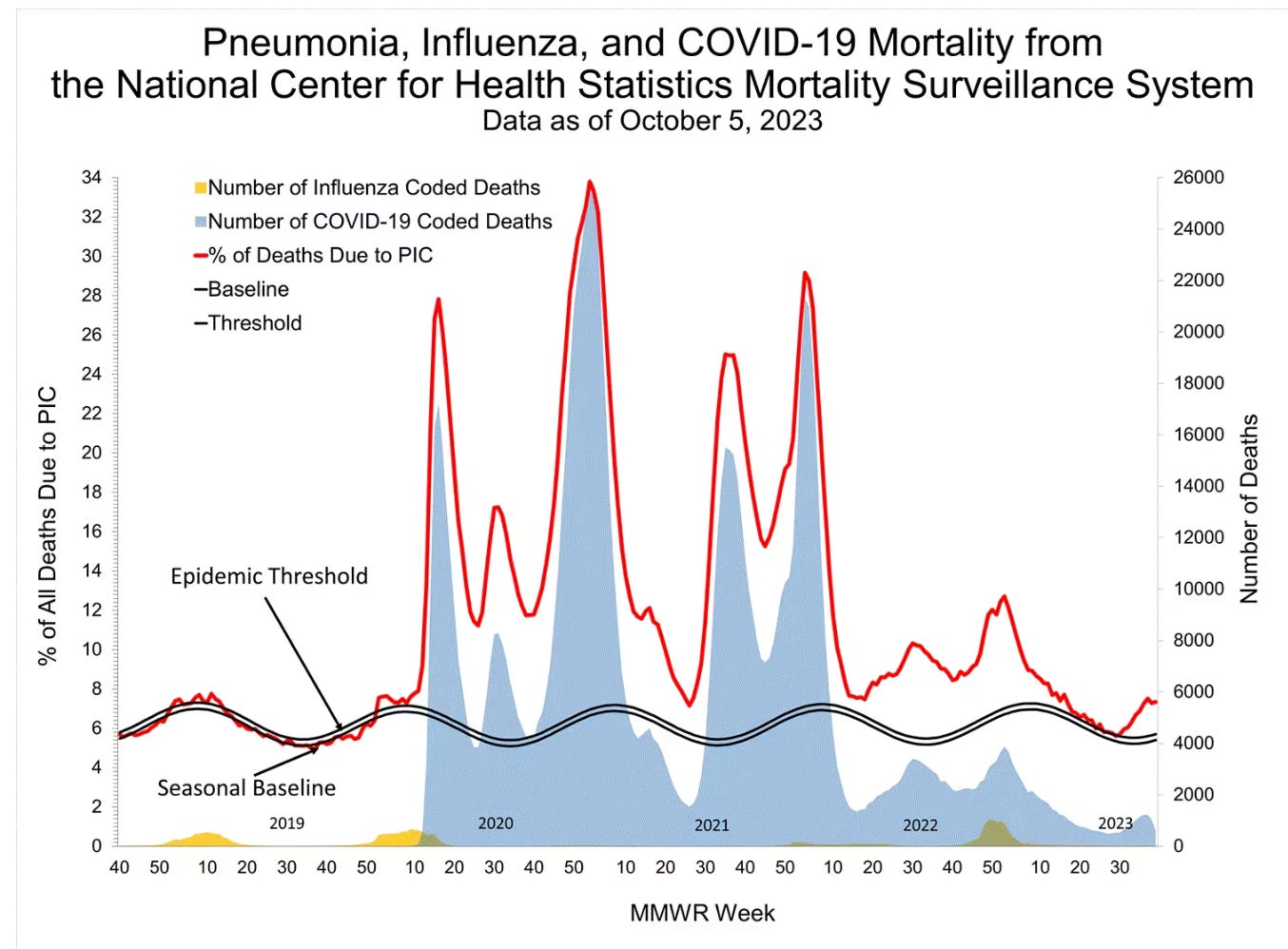
Excess mortality
After hitting a summer low, excess mortality (red line below) is once again above pre-pandemic normals (double black line).
Vaccination
How we fare in the upcoming season is strongly driven by vaccination uptake. The big question this year is whether Covid-19 coverage will match that of flu.
This is where we are right now:
Covid-19: Tracking vaccination rates is tricky now that reporting is not mandated. Last week, the CDC estimated 2% of the eligible population (4 million) have had their fall vaccine thus far. This is on par with last fall's uptake.
RSV: We don’t know about uptake.
Flu: This data isn’t updated until the end of October. In previous years, ~20% of the population had their flu shot by now.
Bottom line
Things are quiet right now, especially with Covid-19 on the decline. This will change in the weeks to come. Be sure to get your vaccinations before Halloween—a safe goal to hit before things heat up. And once that ILI line hits epidemic levels, I strongly recommend putting that mask back on to avoid all types of viruses.
Love, YLE
*this originally said 1 in 4, which was a mistake. 1 in 4 ARE up to date on their vaccine.
“Your Local Epidemiologist (YLE)” is written by Dr. Katelyn Jetelina, MPH Ph.D.—an epidemiologist, wife, and mom of two little girls. During the day, she is a senior scientific consultant to several organizations. At night she writes this newsletter. Her main goal is to “translate” the ever-evolving public health world so that people will be well-equipped to make evidence-based decisions. This newsletter is free, thanks to the generous support of fellow YLE community members. To support this effort, subscribe below:





I’d like to give a huge shout out to Costco, who now has the Novavax vaccine in stock in many of their pharmacies across the country. When I called their pharmacy yesterday, a live person answered their phone, and was happy to book a Novavax appointment for me even though I’m not a Costco member. I get jabbed this afternoon.
Compare this to the multiple phone calls I’ve made to Rite Aid, CVS and Walgreens where customers get stuck in an “automated customer service maze from hell” and often can’t speak to a real person. The few times I was lucky enough to reach the pharmacist, they either had never heard of Novavax, confused it with Moderna, and had no idea whether their company would be receiving it. And www.vaccines.gov is not up to date - the place to get real-time info, unfortunately, remains Twitter, or X, or whatever it’s now called, where there’s currently a #Novavax frenzy.
I have heard (although this isn’t confirmed) that Rite Aid and CVS will eventually get Novavax, but it could take a week or two. Perhaps it’s Costco’s superior internal distribution system that allows it to distribute fresh salmon to stores across the nation that enables it to be first at distributing Novavax.
After this exceedingly pleasant experience, I am planning to reinstate my Costco membership (even though I still have a huge box of unused, tissue-thin toilet paper in the garage from the early days of lockdown).
Also, Novavax plans to release the results of their Hummingbird (kids) study on October 17.
Or put the mask on today. We have a chance to reduce community transmission of ILI. The area under the curve indicates cvd is all around us. If we wait to act, we create the surge.