Oof. Data is starting to roll in on Covid-19 vaccine inequities this fall. And it’s not pretty.
Access. Cost. Outreach. Education. All of these changed once the federal emergency ended in May. Vaccines are no longer purchased or distributed by the government, and funding ran out to support vaccine campaigns. This means the U.S., once again, faces the pre-pandemic privatized and fragmented healthcare and public health systems. And one could argue an even worse system, given the loss of trust.
Unfortunately, our communities continue to feel it disproportionately.
Zoom out: U.S. vs. U.K.
U.S. rates of Covid-19 vaccination this fall are, overall, abysmal. This is especially apparent when we compare it to counterparts like the U.K., where 68% of people over 65 years old are vaccinated (compared to 31% in the U.S.).

Zoom in: Inequities within the U.S.
Within the U.S., vaccination rates are not equally distributed. Disparities were evident last fall and continue this fall:
Race and ethnicity: Communities of color continue to have much lower rates of vaccination. We see this across all sorts of data: national, state (e.g., California), and hyperlocal (e.g., Marin County in California). (Note: Data sources are very different. For example, CDC uses survey data while CA uses immunization records. This means we cannot make comparisons like CA has lower rates than the larger U.S.)
Rurality: A CDC analysis last week found adults in rural areas were less likely to have gotten a Covid-19 vaccine (10%) vs. those in urban (15%) or suburban (14%) areas.
Healthy Place Index (HPI): In California, counties are ranked by an HPI: a measure of conditions that drive health, including life expectancy, income, education, etc. The highest HPI (think high-income) counties have 5.3-fold higher vaccination rates than the lowest HPI counties.
Are disparities widening after the emergency?
Yes.
Epidemiologists in Marin County have started digging into this question.
First, they examined California data to determine differences in vaccination rates by race and ethnicity between last fall and this fall. The gaps in vaccination rates have grown between Latinx and non-Hispanic White (hereafter, “White”) and Black/African American and White residents.
Epidemiologists then looked at uptake this fall among those who got a vaccine last fall, among Marin County residents. This would show whether there are new barriers to accessing the fall vaccine for marginalized groups (rather than hesitancy to get vaccinated).
They found lower fall 2023 coverage by usual resource level and race. Among those who got the vaccine last year, uptake of this year’s fall vaccine was 45% in White residents compared to only 18% in Latinx and 31% in Black residents, and differences between these groups were similar when limited to those 60 years of age and older.
This points to new barriers.
Why does this matter?
The gap between Latinx and White residents who are fully protected is more than twice what it was last year. Same with African American/Black residents. Same with residents of low income.
This means two things:
Those who are more likely to lack access to healthcare are even more likely to be infected and get seriously ill once again.
The commercialization of vaccines has only amplified gaps in access and uptake. This is cause for concern about our national vaccine system during non-emergency times.
Bottom line
When the nation’s health is at stake, we need public health to ensure our resources are fairly distributed and get to those who need it most. The “marketplace” doesn’t do this naturally. In fact, it works against many of our communities. These inequities will continue unless we make big, systemic changes. One would hope that a pandemic would jumpstart these changes, but it seems we are quickly falling back to our pre-pandemic ways.
Love, YLE and the brilliant team at Marin County Health Department (Drs. Matt Willis, LeeAnn Prebil, and Pooja Mhatre)
“Your Local Epidemiologist (YLE)” is written by Dr. Katelyn Jetelina, MPH Ph.D.—an epidemiologist, wife, and mom of two little girls. During the day, she is a senior scientific consultant to several organizations. At night she writes this newsletter. Her main goal is to “translate” the ever-evolving public health world so that people will be well-equipped to make evidence-based decisions. This newsletter is free, thanks to the generous support of fellow YLE community members. To support this effort, subscribe below:







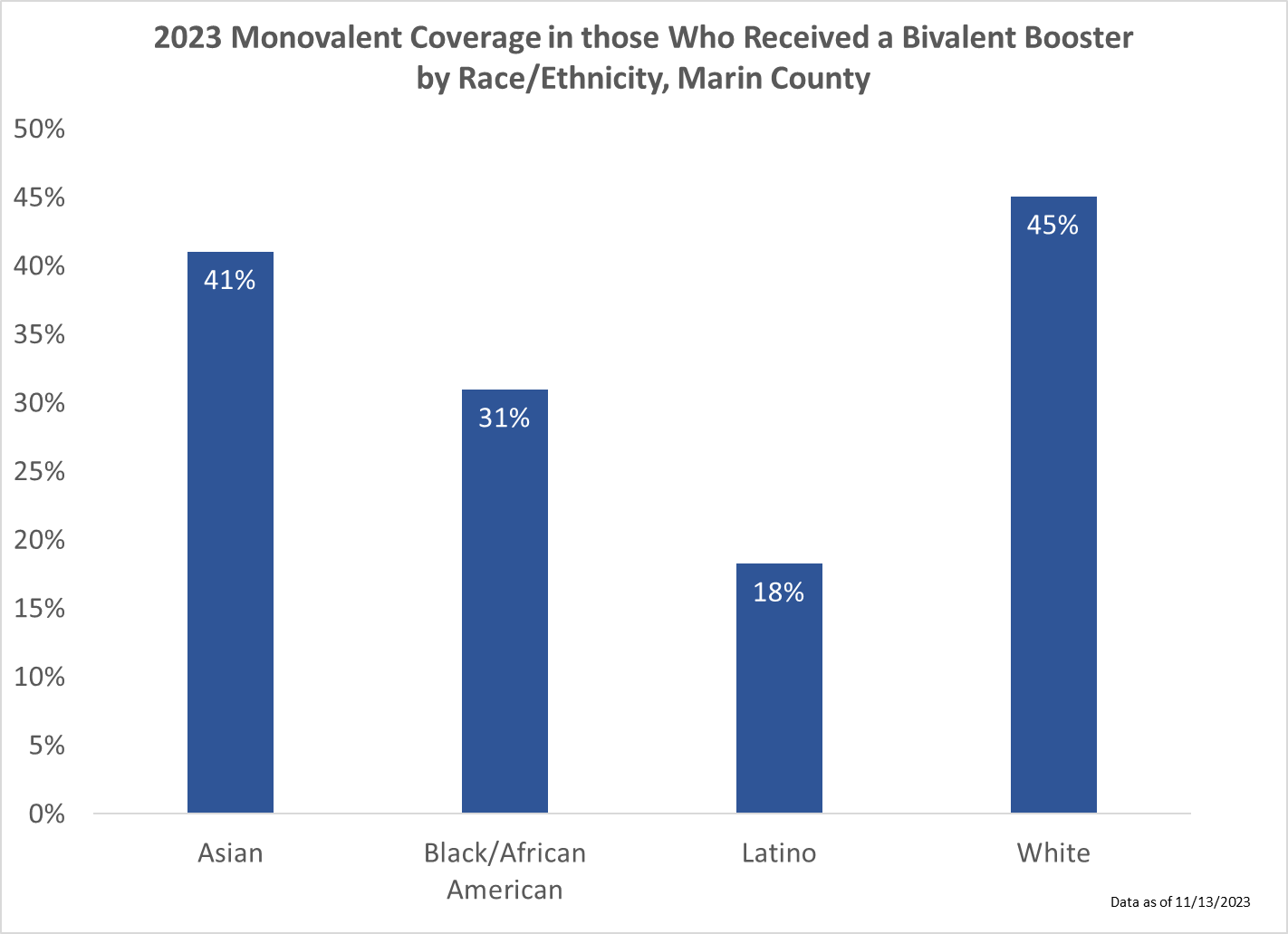
As others have noted, I have not (yet) gotten this year's booster because I caught COVID and was told to wait 90 days before getting vaccinated; sadly, I tested positive on the day I was scheduled to get my booster, so instead of getting vaccinated, I got Paxlovid. I *will* get my booster around New Year's - and I have to wonder how many other people are in my situation and have not gotten boosted yet because of a recent infection, and how that impacts other vaccinations.
As my COVID began to clear up, I contacted my insurance company's advice line to ask when I could get my flu vaccine; it took 3 different people and 5 days to get a call back from my doctor's office, telling me I could get the vaccine any time I hadn't had a fever for 24 hours and felt well. I then began what would become a several month-long quest to get the RSV vaccine - I am under 60 by a couple of years, but immune compromised due to prior cancer treatment, and wanted all the protection I could get. This, also, took several phone contacts and several repetitions of why I wanted it - and why they couldn't approve it, because the CDC guidelines say "60+", with no mention of immune issues - but eventually, I ̶c̶o̶m̶p̶l̶a̶i̶n̶e̶d̶ advocated enough that it was kicked to the immunology department which approved it.
If I, as a reasonably well-education, middle class white woman with insurance that prioritizes prevention, have this much trouble getting vaccinations, I can only imagine what difficulties others, who don't have insurance, who may lack transportation, whose jobs may not give them the flexibility to go to clinics when the clinics are open, etc., may have getting them.
Americans remain stupid.