If you’ve recovered from COVID19, you still need to get the vaccine. Back in May, I gave four reasons why but this is particularly important with Delta and future variants of concern. Here’s why.
Naturally induced immunity
Before Delta, we knew that about 90-99% of people that recovered from COVID19 had detectable antibodies for at least 4 weeks (here, here, here, here, here). For some, protection can last 8 months (because we have 8 months of data, it’s probably more). For others, protection wanes within months. (here, here, here, here, here).
Natural infection can mount a messy response compared to the much more targeted vaccine immunity.
It has to do with how antibodies attach to the virus. Both antibodies (natural and vaccine) block the spike protein from attaching to our cells. One landing target is a specific place on the spike protein called the receptor binding domain, or RBD.
But a recent study found that natural antibodies mainly attach to one region (called E484) on the RBD while vaccine antibodies can attached to many regions. This can be problematic for natural immunity as the virus mutates and regions on the RBD change. Because vaccine antibodies can attach to many regions, the vaccine antibodies have more flexible landing options and thus provides better protection potential as the virus changes.
We saw better protection with other variants of concern
A small study took blood samples among healthcare workers at three time points:
After “natural” infection;
Before vaccination;
After vaccination.
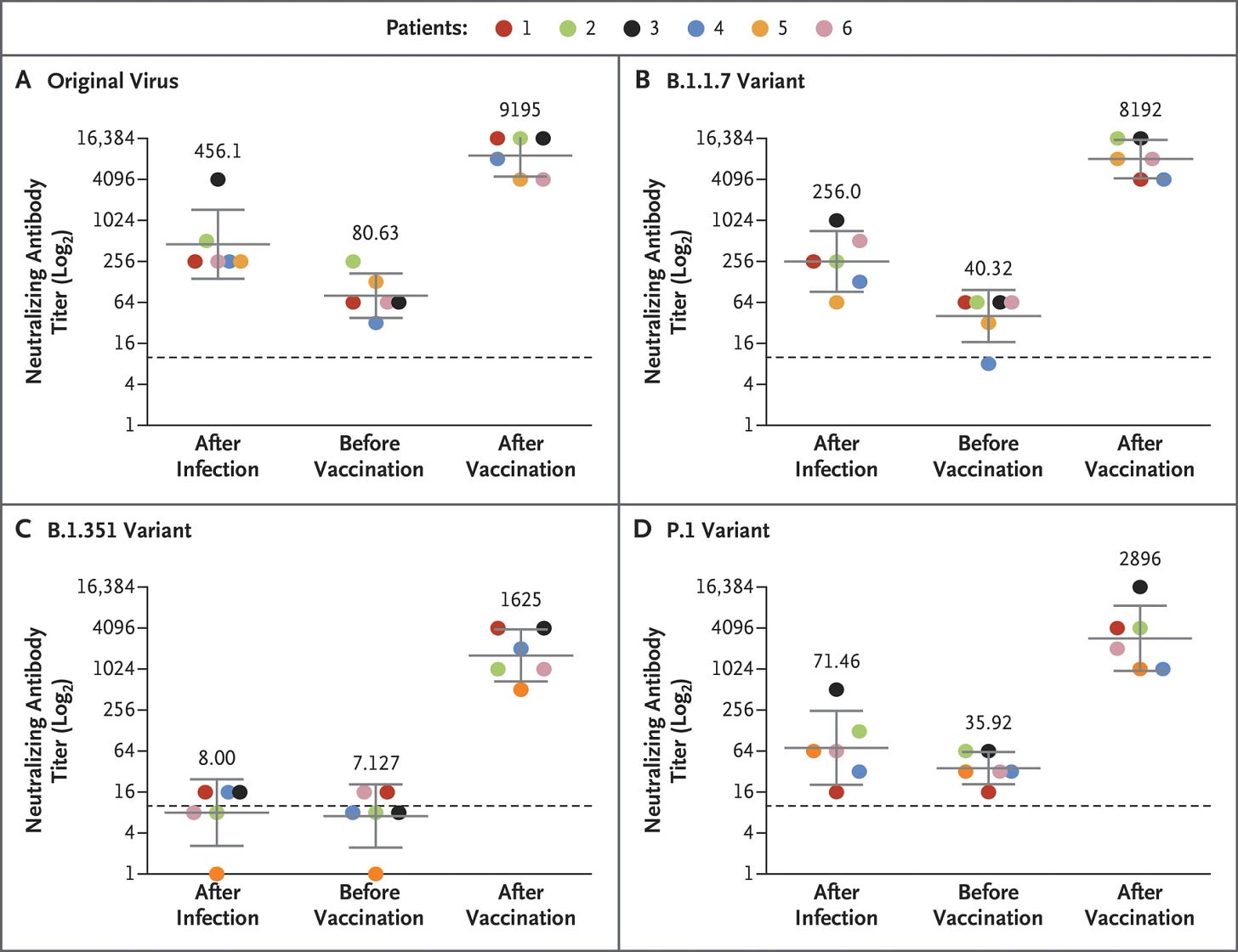
Then, scientists “infected” the blood samples with variants of concern to see how well antibodies responded.
Vaccines were better at increasing the number of neutralizing antibodies than natural infection. In other words, vaccinated had more soldiers.
Vaccines also had more neutralizing antibodies against B.1.351 (variant first detected in South Africa) and P.1. (variant first detected in Brazil) compared to natural immunity.
We’ve also seen this in population-level studies (not just petri dish studies). Last week an important study from the CDC looked closely at reinfection rates. Using a pre-existing database, scientists found 246 Kentucky residents who were infected in 2020 and reinfected in 2021 (May 1–June 30, 2021-note before Delta). In the same database, scientists then found similar people (age, race/ethnicity, etc.) with the counterintuitive: infected in 2020 but not reinfected in 2021. Then the scientists compared the vaccination status of the two groups.
Reinfection was 2 times more likely among unvaccinated compared to vaccinated. The naturally induced immune response was just not working as well as the vaccine induced immune response.
We have preliminary evidence that Delta makes reinfection more common
The Public Health of England found that the reinfection rate is worse with Delta compared to previous variants. This was particularly true when there were more than 180 days between the first and second exposure.
Symptoms for reinfection
And just because you had a previous case, doesn’t mean you’ll fare any different. In fact, one small study found people fared worse during reinfection, particularly if the first infection was asymptomatic or mild.
Bottom Line: The immune system is incredibly complex but we are slowly getting more and more evidence that natural immunity is not as effective as vaccine immunity. If you’ve recovered from COVID-19, you still need to get vaccinated to continue to fight against the ever changing virus.
Love, YLE







Why are we not seeing reinfection statistics? We have been seeing comparisons between the recovered vaccinated vs recovered unvaccinated. But have seen nothing of unvaccinated reinfection vs. vaccinated breakthrough cases with both case numbers or hospitalizations/deaths. We know that antibodies are not the only indicator of immunity, and yet, scientists are using antibody studies to dictate who is protected and who is not. The chart above from the UK shows that reinfection with delta vs. alpha was 1% of cases vs 0.2% of cases, that seems like it is less than breakthrough cases with the vaccine. Additionally, including a study looking at 5 patients in a skilled nursing facility is not a reliable study to support anything. The scientific community is not providing enough data about reinfection, and those who are supporting that vaccines are more comprehensive than natural immunity with subpar data ie. only looking at antibody response, using small studies (of 5 people) are perpetuating theories based on lacking info.
https://www.nature.com/articles/s41586-021-03647-4
First, thank you thank you thank you for all you do. I read all your posts and point everyone I know to you. I jumped on to substack to specifically ask a question about reinfection only to find it was your post today. Sadly, my kids are both infected with covid despite masking everywhere we've gone all summer long (we live in Texas). I was hoping we could get a brief reprieve once we're out of quarantine and let them do things we haven't been doing for the last 1.5 years. I'm in literal tears that this isn't the case. But I'm also feeling so much better about switching them last minute to a school that follows CDC guidelines on masking (they showed their first symptoms of covid 1 day after I made the switch official).