Today we got our first Omicron lab data! A week and half since Omicron broke the news. Just beautiful. As the scientist of the study said, “If I don’t die from the virus, I’ll die of exhaustion”. We’re getting more and more epidemiological data, too. Together they give us a dense, but clear(er) picture of Omicron.
Here we go…
Does Omicron “escape” our vaccine immunity?
Our first Omicron lab study was released today. A group of South African scientists, led by Dr. Alex Sigal, mixed a live virus with blood samples of 6 people who had 2 doses of Pfizer. They also mixed the virus with blood samples of 6 people with the 2-dose series and a previous infection. (South Africa has not authorized boosters yet, but this is a good proxy).
In order to assess vaccine “effectiveness,” the scientists counted the number of neutralizing antibodies that attached to Omicron. Neutralizing antibodies play a significant role in our protection against infection, as they quickly recognize the virus and destroy it. Importantly, the virus is destroyed before entering cells and, thus, cannot replicate. Because it can’t replicate, the person doesn’t get infected and doesn’t get disease (i.e. symptoms). The more neutralizing antibodies we have the better.
In this study, the scientists assessed how Omicron enters our cells and how many antibodies respond to Omicron compared to the original SARS-CoV-2 virus. What did they find?
The virus is using the same door into our cells (called ACE2 receptors) as before. This is very good news because it means our tools (like vaccines) are still useful. If the virus found a different door, this may not have been the case.
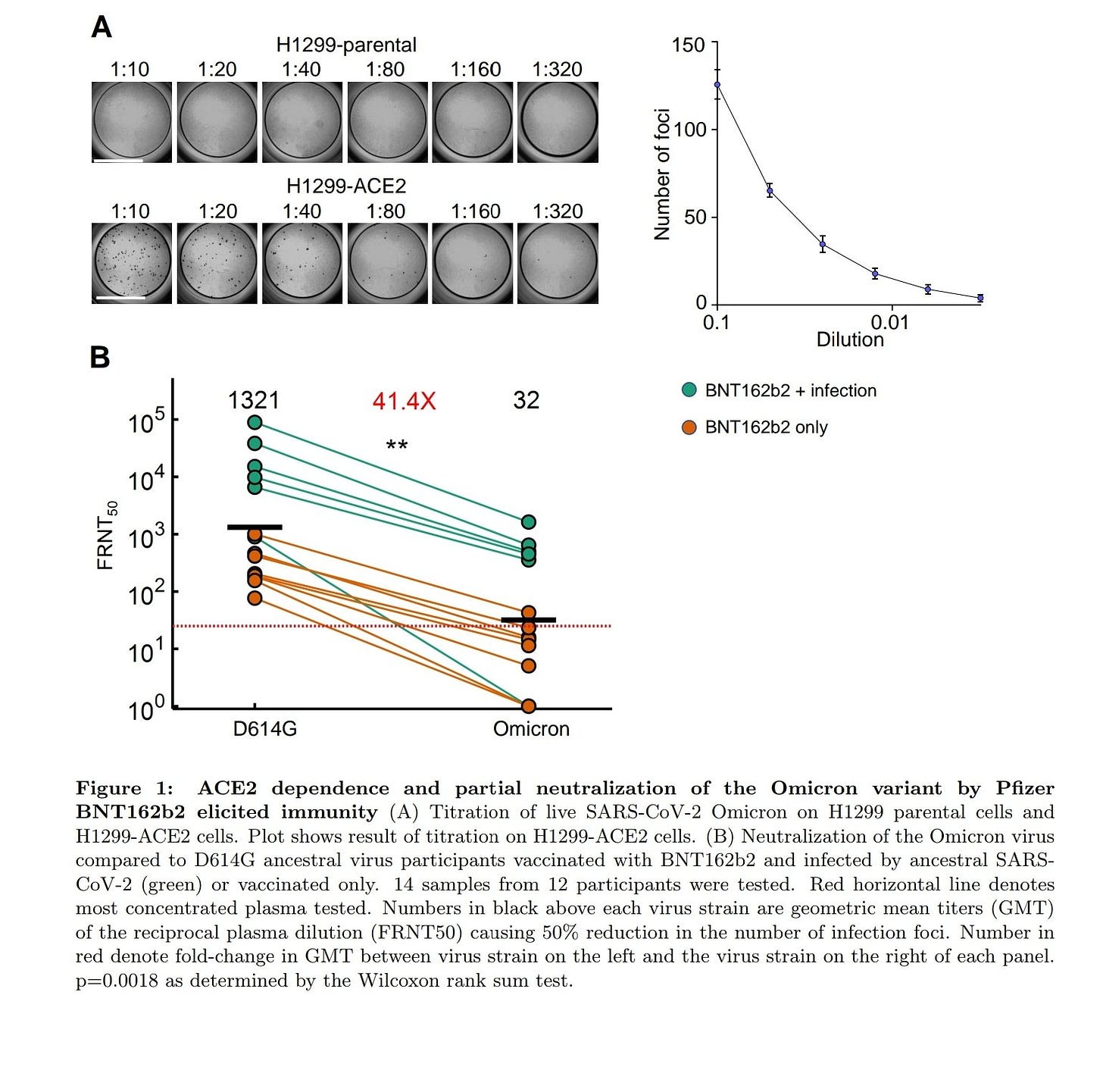
The virus is making a smarter key to that door. Panel B in the figure below highlights the main finding of this paper:
Among people with the 2-dose Pfizer series (orange dots), neutralizing antibodies took a significant hit —40 fold reduction— with Omicron compared to the original virus. This is far higher than we’ve seen with any previous variants of concern (Delta had a 5 fold decrease; Beta had a 8 fold decrease). But, honestly, Omicron’s decrease is not as bad as some expected.
Among people with the 2-dose series + previous infection (green dots), neutralizing antibodies took a hit from Omicron but are still relatively high.
This means we’re going to see an increase in breakthrough cases, especially among those with only the primary series. But this study gives me great hope that our boosters will help protect against Omicron. In addition, and importantly, neutralizing antibodies are not our only defense. We have other antibodies, B-cell factories, and T-cells (I explained them here) that will also help protect against severe disease and death. It will take time and more data to determine if we need an Omicron-specific booster.
Does Omicron increase transmissibility?
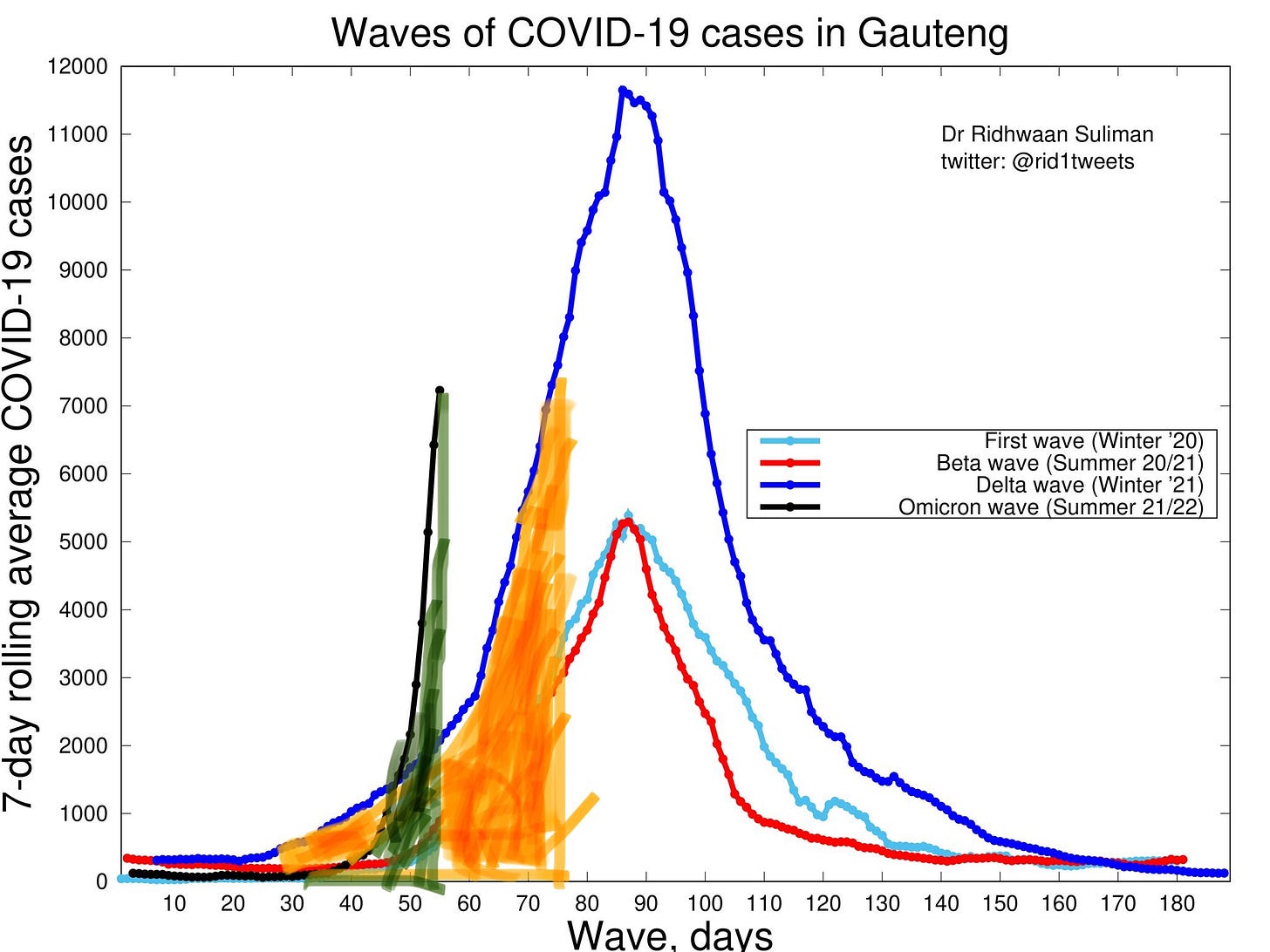
Cases continue to exponentially increase in South Africa. Their 7-day average passed 10,000 yesterday for the fourth time during this pandemic. Cases also continues to climb in the epicenter of Gauteng too.

The R(t)—a measure of contagiousness— in South Africa is holding steady at an incredibly high rate: R(t)= 2-3. The graph below shows Omicron having the highest R(t) in the history of the pandemic in South Africa. This means that there’s far less in Omicron’s way, like immunity, than before. This makes sense now with the lab data.
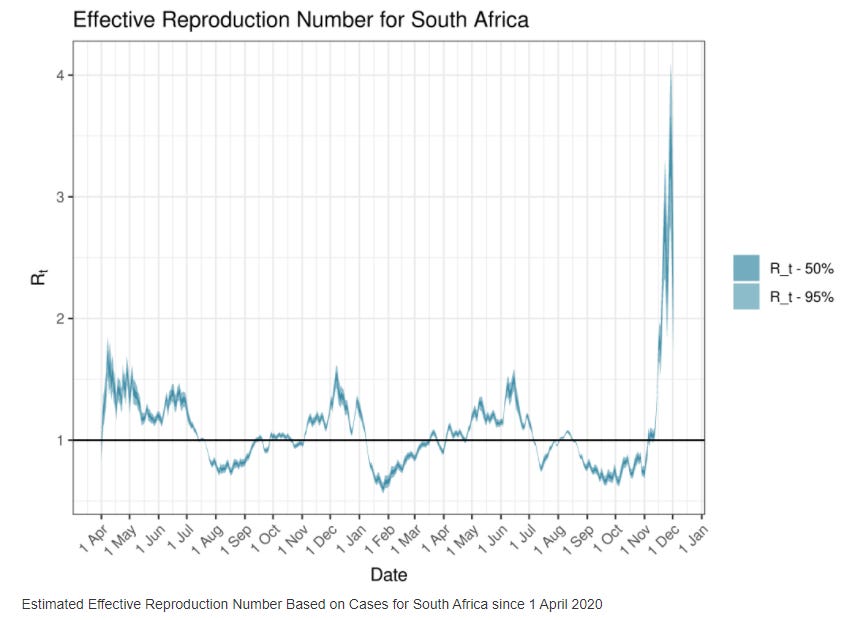
There was hope that Omicron might not spread as fast in Europe or the States. We wouldn’t necessarily see the same rate of spread as in South Africa because high rates of Delta and vaccination would be in Omicron’s way.
We’re starting to get data from the UK and it’s really not looking good. On Dec. 2, 2% of their PCR swabs were positive for Omicron. This is compared to less than 0.01% positive PCRs on Nov 20. Mathematical models estimated an R(t) of 3.47 in the UK right now. This is likely an overestimation, but even the best case scenario (i.e. lower bound) of the R(t) is concerning at 2.75. This tells us that high levels of Delta and/or immunity are not stopping Omicron in the UK. And it probably won’t stop Omicron in the United States either. We need to continue to watch this, but this is not a great start at all.
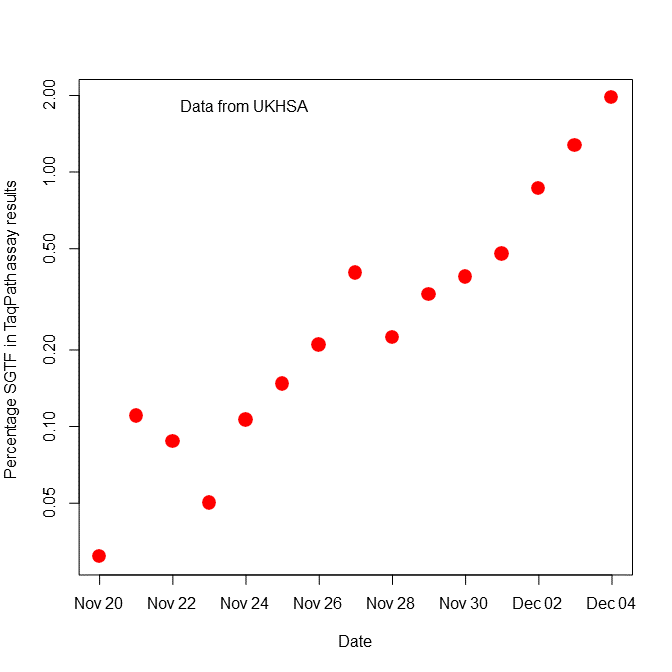
Does Omicron increase severity (hospitalization or death)?
Omicron is causing a lot of infection very quickly across different landscapes. But infection is very different than severe disease or death. So, what’s happening to people that do get infected?
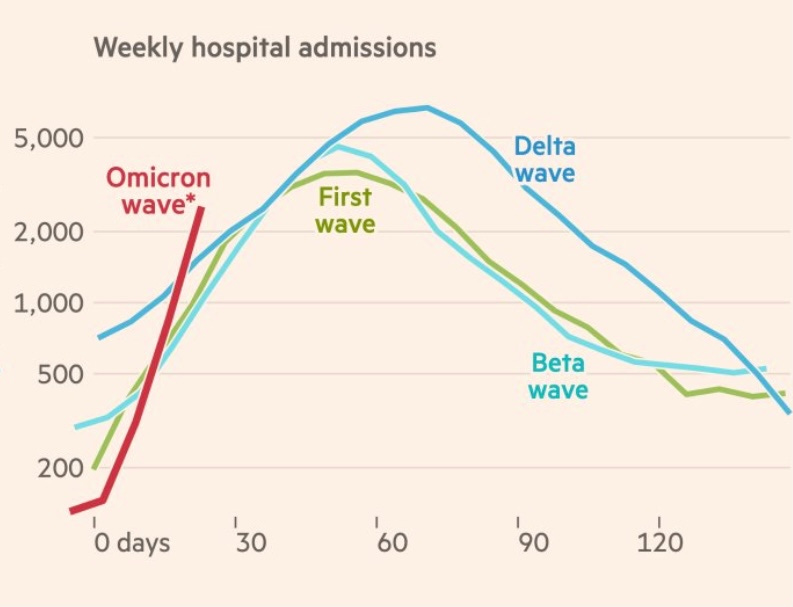
In Gauteng, hospitalization of COVID19 cases in South Africa’s epicenter is increasing exponentially. And it looks like it’s accelerating at the same rate as previous waves.
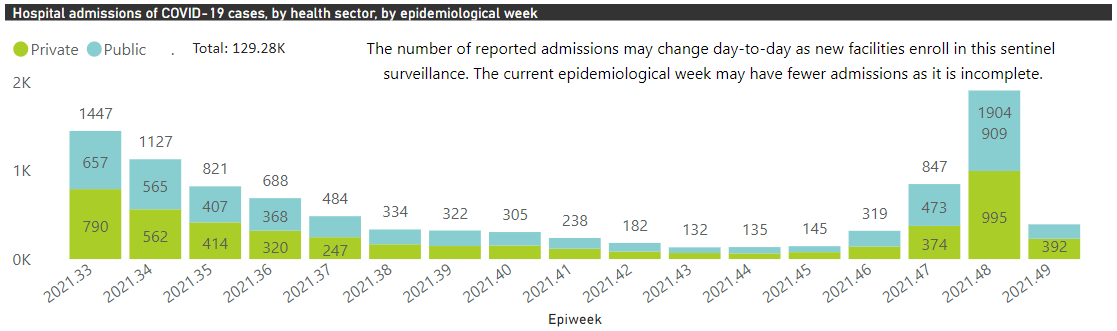
But a report from one of these hospitals provided more context about individual hospitalizations over the weekend. Among a sample of 42 COVID patients in the hospital on Dec. 2, most were hospitalized “with COVID19” not “for COVID19.” Among the 42 patients, 9 (21%) had a diagnosis of COVID19 pneumonia. Among the 9 pneumonia patients, 8 were unvaccinated and 1 was a child. There were 4 patients in high care and 1 in the ICU.
This is a very important on-the-ground perspective. But it is still a very small piece of the puzzle. It is far too early to conclude that Omicron is mild; there are a variety of factors tangled up with each other:
Are we seeing mild cases because vaccines are working or because Omicron is a less severe disease? We can have a virus that leads to mild cases, but isn’t less severe.
Are the majority of cases mild because South Africa has a relatively younger population than, for example, the United States? Extrapolating real-world data from one place to predict how we will do in another place is not straightforward.
Is Omicron growing too quickly, so we don’t have enough data yet? This may seem counterintuitive, but in a fast-growing epidemic, the proportion of cases is actually smaller than the proportion of cases in a slower growing epidemic. I tried to show this phenomenon in the figure below. At the same point in the wave, the proportion of Delta cases (orange highlight) was far higher than the proportion of Omicron cases (green highlight). This factor alone could cause an unusually low proportion of hospitalizations at first. We have to see what happens when this denominator gets bigger and bigger.
We may already be seeing this in the data, too. The acceleration of patients in the ICU and ventilators is faster than the previous Delta wave.
We are also mixing individual-level implications with population-level implications. Immunity may largely protect us against Omicron. But people do still end up in the hospital. Four out of 42 patients (9%) in the South Africa hospital needed intensive care. A small percentage can add up quickly when we are talking about an incredibly fast virus moving through 330,000,000 people in the United States.
And finally, something that I haven’t even see get mentioned is morbidity. Long COVID is less prevalent among vaccinated (see my previous post here), but it does still happen. Just ask anyone with long COVID. You don’t want it.
Differentiating all these factors is incredibly important to determining whether Omicron is more severe. Untangling will take time. And we haven’t had that time yet.
Bottom Line
There’s a good chance Omicron will outcompete Delta in the United States. This coupled this with the high unvaccinated rate and lab data showing partial vaccine immunity will result in a substantial Winter wave. The rate of breakthrough cases will be higher, but I’m hopeful that boosters will largely keep people out of the hospital.
We’re all exhausted. The scientists. The healthcare workers. The parents. The pharmacists. The teachers. Everyone. But the virus isn’t. And it won’t be until we all take it seriously. Wear a good mask. Ventilate spaces. Test, test, test. And, for the love of all things, go get your vaccine and/or booster.
Love, YLE
A few random notes:
The U.S. Chambers of Commerce invited me back to answer more Omicron questions on Thursday at 4pm Eastern. Register here. It will be recorded, too.
Those looking for a good mask can start here— a fantastic database of masks tested for effectiveness. Here is the kids’ mask database.
Yes, antigen tests work against Omicron. They test for another part of the virus—they do not test against the spike protein. They still work, so please use them.
“Your Local Epidemiologist (YLE)” is written by Dr. Katelyn Jetelina, MPH PhD— an epidemiologist, biostatistician, professor, researcher, wife, and mom of two little girls. During the day she has a research lab and teaches graduate-level courses, but at night she writes this newsletter. Her main goal is to “translate” the ever-evolving public health science so that people will be well-equipped to make evidence-based decisions, rather than decisions based in fear. This newsletter is free thanks to the generous support of fellow YLE community members. To support the effort, please subscribe here:




Thanks—every single post,thanks! If you have a moment, I was confused by this statement: “We can have a virus that leads to mild cases, but isn’t less severe.” Does that means mild cases on an individual level (generalized, of course), but potentially still severe impacts at a broader scale (hospitals filling up and having to ration care, etc.)? Or am I missing the point? Thanks!
Thanks for a great summary, and for acknowledging Long Covid. I always see Long covid as an afterthought in many articles(at best). It would be great if you can share how the scientific community is doing on understanding the causation of Long Covid. We have a bias in the medical establishment that puts more resources towards heart attack and sudden illness rather than chronic illness. I have had a long covid since mid-2020 and it is indeed something that you want to avoid. Not saying morbidity should be treated on par with mortality but it needs a separate lens altogether