When will hospitalizations start decreasing?
Currently, 21 states/territories have administered enough shots to cover at least 40% of the population. So, when are we going to see an impact on COVID19 hospitalizations?
Short answer: When ~56% of the population is fully vaccinated.
Here is the data-driven, evidence based answer…
Individual vs. Population
This distinction is key.
On an individual level, we know vaccines protect against severe disease (i.e. hospitalizations and deaths). In the “real world”, vaccines are 95% effective in keeping you out of the hospital (in clinical trials this number was 100%).
On a population level, this is more complex. The impact of vaccinations (on a population level) is much more difficult to see than on an individual level. That’s because there are three competing demands happening at once:
Vaccinations (which is good);
Wide-spread transmission in some areas (which is bad); and
Variants of concern (which is bad).
Here are some examples in the United States…
California
Vaccination rate: Moderate (31% fully vaccinated)
74% of 65+ are vaccinated
Transmission rate: Moderate (40 cases per 100,000)
New variants: Low (B.1.1.7. accounts for 43% of cases)
What does this combination result in? Hospitalizations are decreasing, but also are cases. In fact, they nearly mirror each other. The age distribution for hospitalizations reflect the distribution in September (green and red bars look about the same). Not enough people are vaccinated, especially among 65+, to see a population-level impact on hospitalizations.
Michigan:
Vaccination rate: Moderate (32.5% fully vaccinated)
75% of those aged 65+ are vaccinated
Transmission rate: High (432 cases per 100,000)
New variants: High (B.1.1.7. accounts for 67% of cases)
What does this result in? Hospitalizations mirroring cases. But, the age distribution looks different than their last peak. This is likely due to a combination of vaccines (making those red bars smaller) and high transmission/variants of concern (making those green bars bigger).
Vermont
Vaccination rate: High (37.9% fully vaccinated; Leading the country in vaccinations)
Transmission rate: High (106 cases per 100,000)
New variants: Low (B.1.1.7. accounts for 46% of cases)
What does this result in? Hospitalizations mirroring cases. But, the age distribution looks different than in early December. This is likely due to a combination of vaccines (red bars smaller) and high transmission/variants of concern (green bars bigger).
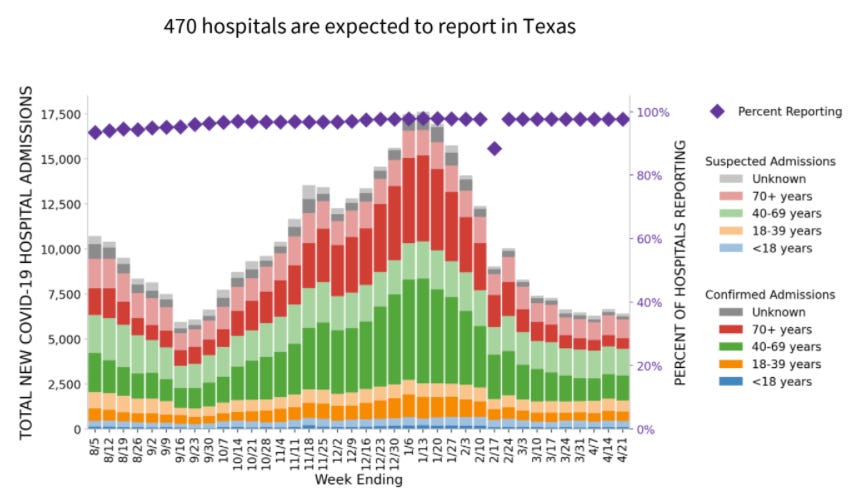
Texas
Vaccination rate: Low (27.5% fully vaccinated)
Transmission rate: Substantial (70 cases per 100,000)
New variants: High (B.1.1.7. accounts for 69% of cases)
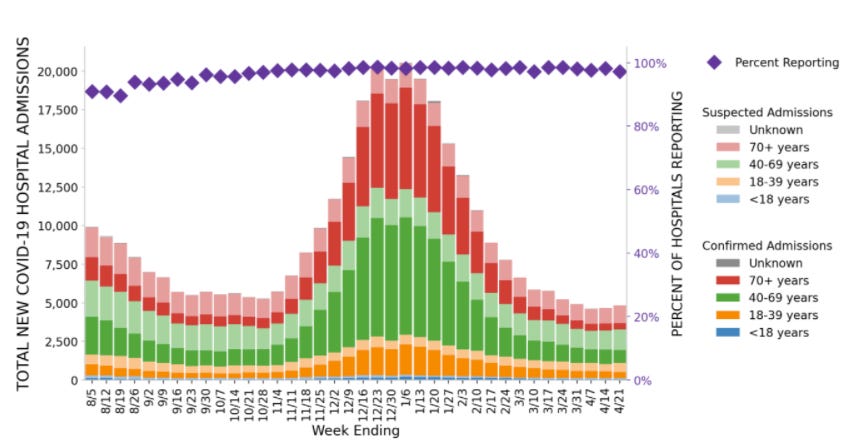
What does this combination result in? Looks a whole lot like CA. The age distribution of hospitalizations looks the same as it did in September. Not enough people are vaccinated to see population-level impact.
Case example from Israel
The picture in the States are muddled. So, epidemiologists are using Israel to inform policy. Israel is the global leader in vaccinations.
Context: Transmission rate was HIGH in Israel during their vaccination campaign. Also, B.1.1.7. hit them hard too once they got transmission under control. So, I would say Israel was more reflective of Michigan’s situation. However, Israel was vaccinating at incredibly high rates.
A study came out two weeks ago and I just love how they presented their data.
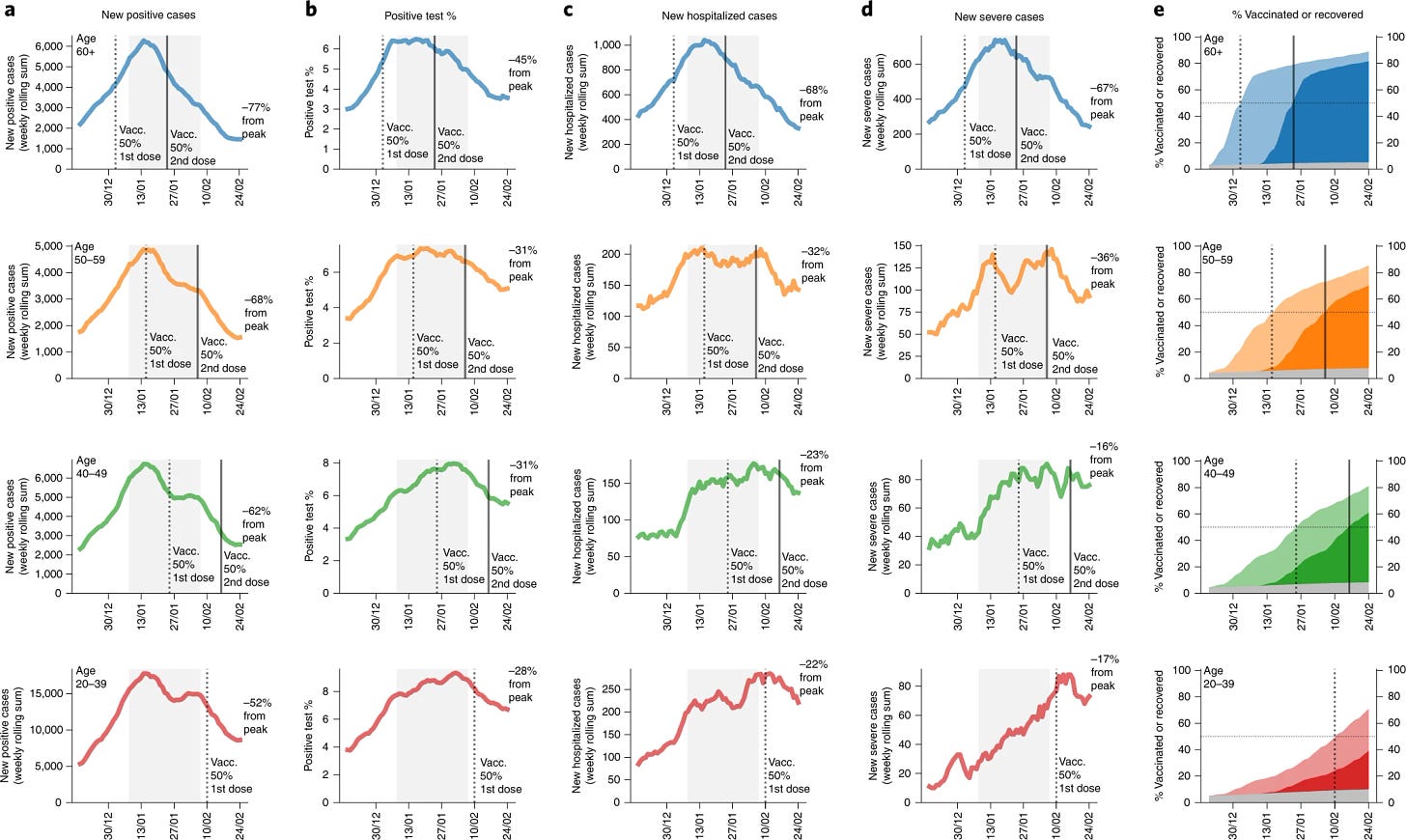
Below is one figure key figure of theirs. Each row is a different age group (blue=60+, orange 50-59, green 40-49, and red 20-39 years). The solid vertical line in each graph represents when 50% of that age group was fully vaccinated.
Focus on column C (new hospitalizations) and column D (new severe cases). It’s clear that hospitalizations started decreasing for each age group once 50% of that group (actually 56% to be exact) was vaccinated
Bottom Line
We need more people vaccinated in the United States to see a clear population-level impact on COVID19 hospitalizations. It’s coming (slowly but surely).
Love, YLE