Driven by Omicron sub-variants, country-level hotspots are now peppered across the globe. Yesterday, the WHO reported cases are on the rise in 110 countries, causing overall global cases to increase by 30% over the past two weeks. Of course, these numbers and country-level comparisons are only as accurate as testing and reporting.
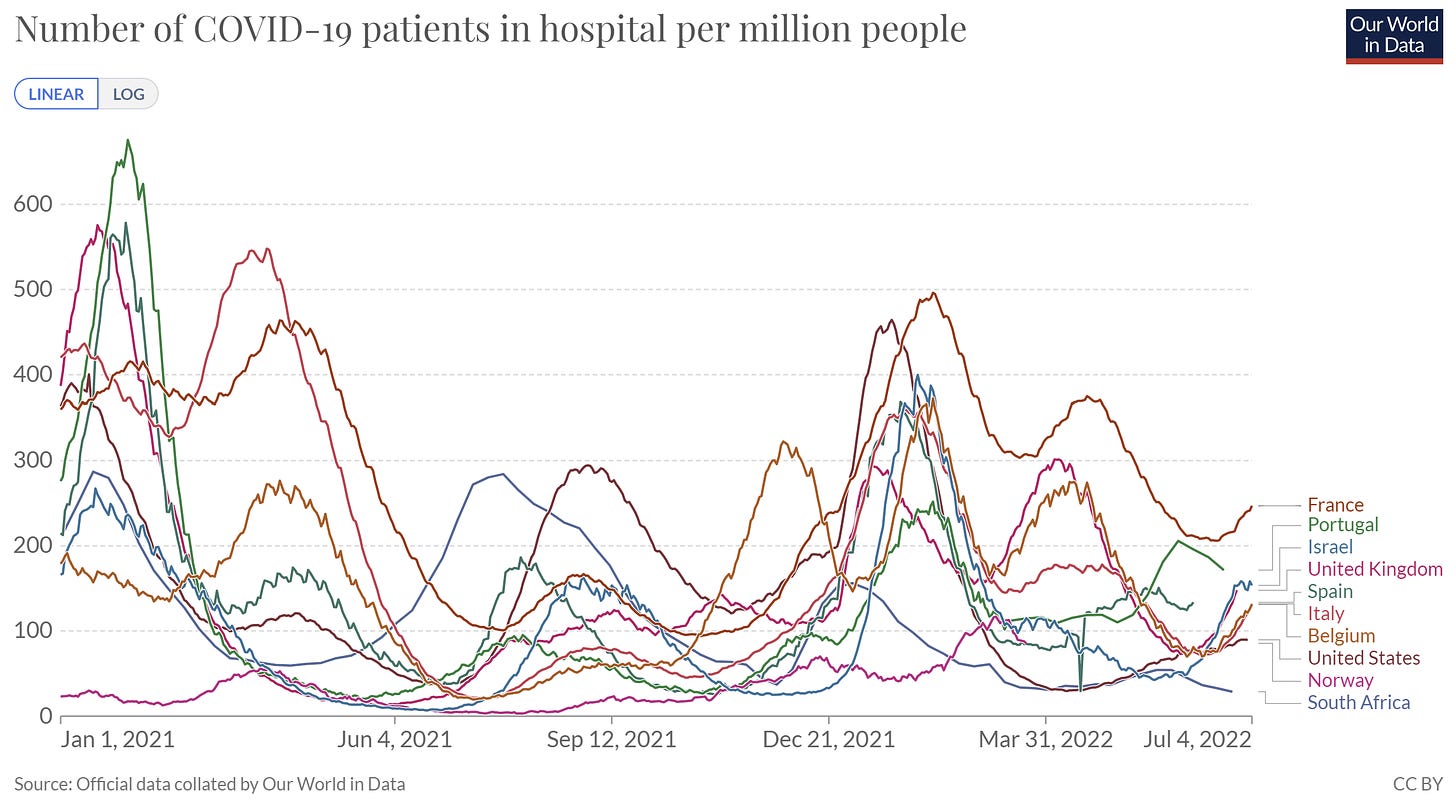
In Europe, BA.4/5 is driving a case surge. Hospitalizations in Portugal finally peaked and are well on their way down. Hospitalizations in other European countries continue to rise, though.
In the U.K., it’s clear that hospitalizations rising are both with and for COVID19. The distribution seems to be stubbornly consistent since a switch during the first Omicron wave last winter, when hospitalizations for COVID19 took the lead.
In India, all eyes are on a new variant: BA.2.75. After first being discovered at the end of May, it quickly took hold and now accounts for 25% of cases, with most samples reported from Maharashtra (Mumbai). There is sparse testing data in India (see the grey bar charts in the figure below), but BA.2.75 appears to be outcompeting BA.5 and BA.2 (with a growth advantage of 17% thus far). This means it has the potential to cause a wave and is important to follow. BA.2.75 cases have been identified in other countries, like Australia, New Zealand, U.K., and Germany, but remain low at this time.
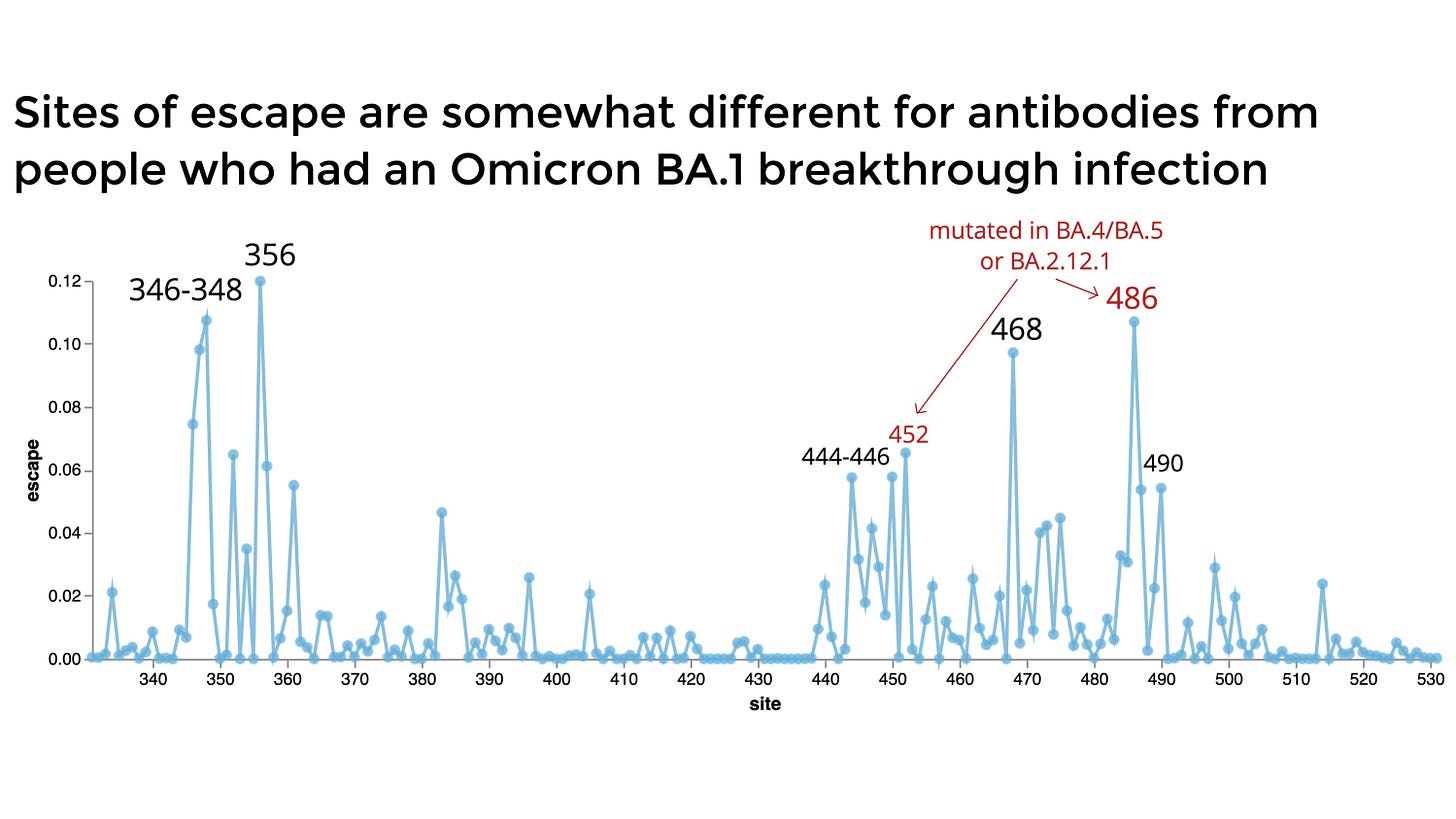
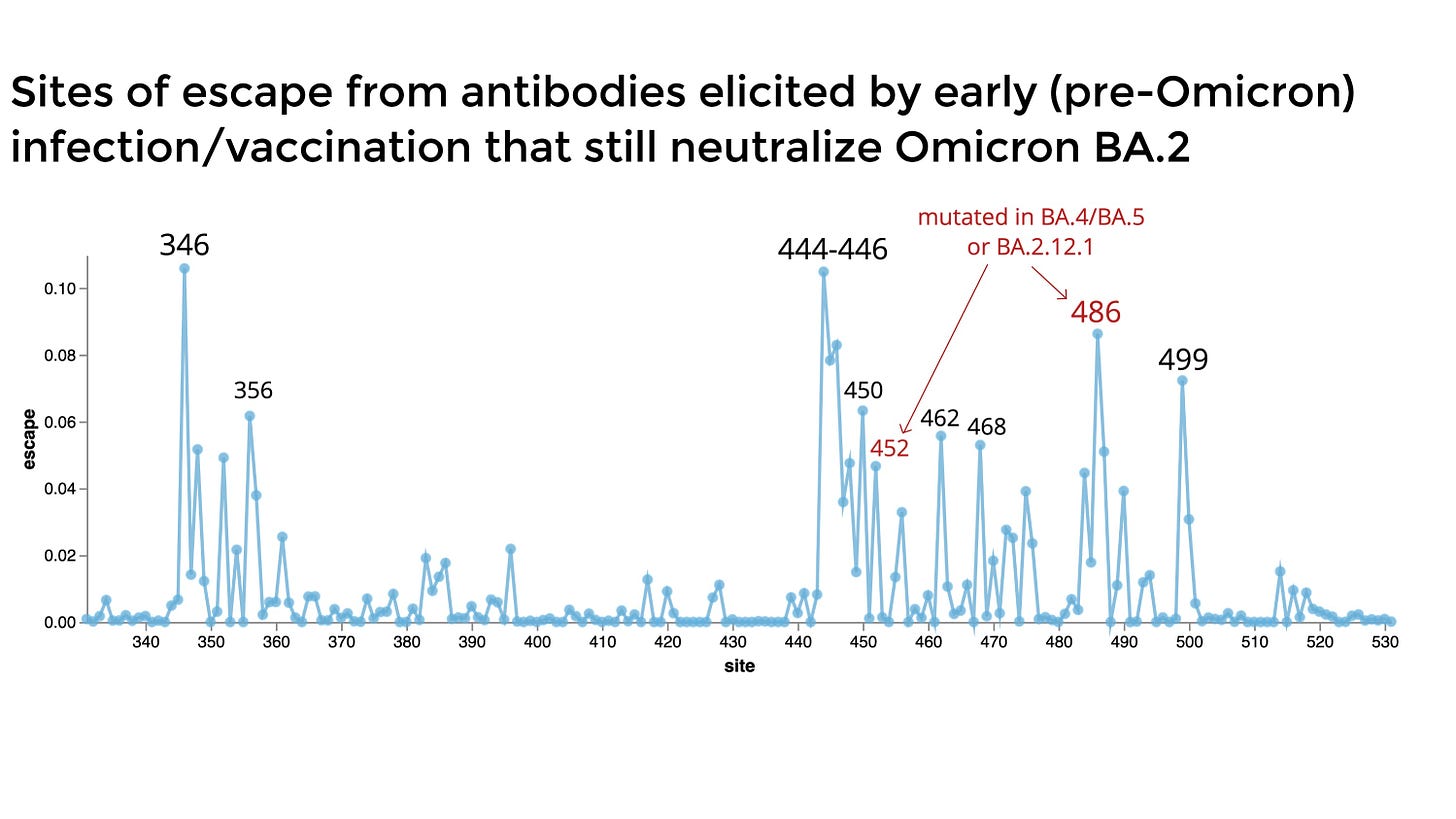
BA.2.75 carries eight additional mutations on the spike protein compared to BA.2. There are two mutations in particular that are cause for concern: G446S and R493Q. G446S is at one of the most potent sites of escape from antibodies. As the Bloom Lab interestingly pointed out in the figure below, BA.2.75’s impact will be dependent on infection history. Among those with a previous BA.1 infection, the probability of immune escape at spot 446 (and thus infection) is lower than those without a previous infection.
A few more thoughts on this sub-variant:
Let’s be glad the mutation G446S isn’t on BA.5. If it was, this subvariant could make an even bigger impact. If BA.2.75 does take off, it will be co-circulating with BA.5, so keeping a close eye on recombinants will be important.
This makes the fall booster conversation interesting. Last week, the FDA authorized a BA.4/5 vaccine formula. However, one could make the argument that the original BA.1 vaccine formula would be better with this BA.2.75 news. But, chasing variants is never going to work. Our goal should be broaden protection. An Omicron vaccine will do that, regardless of the sub-variant circulating.
United States
In four short months, four Omicron sub-lineages have come and gone in the U.S. Currently, BA.4/5 made a fast entrance and now accounts for more than 70% of tests. Interestingly, BA.4 stopped (or substantially slowed) growth, so this is really now a story about BA.5. It’s not clear whether BA.5 will result in a wave in the U.S. given our BA.2.12.1 history that other countries did not experience. If we do get a BA.5 wave, it would start about now, so all eyes are on epidemiological trends.
The U.S. holds a steady state of ~100,000 reported cases per day. This equates to about 1M “true” cases per day, using back of the napkin math. (At the height of the first Omicron wave, we experienced ~3.9M true cases per day). The steady state is reflected in national wastewater with plateauing trends across every region.

Interestingly, our national test positivity rate (TPR) continues to increase and is at a high rate of 17%. Anecdotally, it feels like more and more people are testing positive, too.
The disagreeing patterns between cases/wastewater and TPR could mean that a wave is about to come (historically, TPR trends upwards first). Or it’s a reflection that cases are just a terrible measure of community transmission. Lack of testing, lack of reporting antigen tests, and biased testing (some groups are more likely to get tested than others) are creating really weird trends in metrics. This begs the question: How do we detect a wave at this point in the pandemic?
Hospitalizations continue to creep up and, on average, 389 Americans are dying each day. Severe disease will continue to occur. As the Kaiser Family Foundation reported, in some states, 3 in 4 people are not up to date on their COVID-19 vaccines (this figure does not include the 4th dose). Also, as we just saw in Portugal, vulnerable groups like the elderly are at risk from high transmission, even if vaccinated. While incredibly tragic, hospitalizations and deaths do remain below any previous peaks, which is progress.
Bottom line
BA.5 is impacting countries across the globe. It’s story in the U.S. is yet to be determined. It’s important to note, though, that we already have a very high, steady level of transmission. In addition, SARS-CoV-2 continues to mutate so quickly that we start talking about the next variant (BA.2.75) before the current wave peaked.
Love, YLE
“Your Local Epidemiologist (YLE)” is written by Dr. Katelyn Jetelina, MPH PhD—an epidemiologist, biostatistician, wife, and mom of two little girls. During the day she works at a nonpartisan health policy think tank, and at night she writes this newsletter. Her main goal is to “translate” the ever-evolving public health science so that people will be well equipped to make evidence-based decisions. This newsletter is free thanks to the generous support of fellow YLE community members. To support the effort, please subscribe here:









I really appreciate your blog posts, especially about COVID. With public interest waning and with a decreased demand or public interest for updated information, it is becoming harder to find science based information I can count on. So thank you so much for your work; I am very grateful!
I really appreciate this as it’s become impossible to get accurate information with the lack of testing and most departments of health ramping down.
I just read that “ pandemic fatigue “ is overstated in the media and the people most at risk— front line, essential workers, people without paid sick leave, etc— are still very much interested in accurate information and how to keep themselves safe. Kaiser Family Foundation polls consistently show more people are still concerned but perceive that “back to normal “ is the norm, so they/ we think we’re in the minority of people who still recognize that the pandemic isn’t over. Information is power, and your information is so crucial. Thank you!