There’s been a ton of meetings re: COVID19 boosters. VRBPAC met last week (here are my cliff notes). FDA made their decision yesterday. ACIP (the external advisory committee to the CDC) met today. The evidence from all these meetings are pretty clear: boosters are safe, effective, and needed for some. This weekend it will be “legal” to mix vaccines too. But everyone has one question…
Which booster should I get?
When deciding to mix or match a booster, you should weigh benefits with risks. This benefit/risk ratio depends on age, sex, vaccine type, and risk for COVID19 disease. Thanks to the ACIP meeting today, we got some new data that can help drive your decision…
Benefits to Mixing
At the ACIP meeting, scientists of the landmark mix and match study presented their data. I wrote about this study last week. Briefly:
The most benefit was for those with a primary J&J shot. A Moderna booster gave the greatest benefit (56.1 fold increase in IgG; 76.1 fold increase in neutralizing antibodies). Pfizer also worked very well (32.8 fold increase in IgG; 35 fold increase in neutralizing antibodies).
After the primary Moderna series, there was equal benefit from either a Moderna or Pfizer booster.
After the primary Pfizer series, the greatest benefit was from a Moderna booster. But a Pfizer booster helped a lot too.
There is a level of uncertainty about what combination is the best, though:
We don’t know why mixing leads to increases of antibodies for some groups but not all. For example, is J&J highly boosted by Moderna because..
…Moderna has such a high original efficacy?
…they are different biotechnologies? Theoretically mixing an adenovirus vaccine (J&J) with a mRNA vaccine (Moderna) could give your immune system more ways to identify the virus, and thus more effective.
… of the order? The “primer” or the original vaccine is important. Maybe this partially explains why JJ then Moderna is better than Moderna then JJ.
Scientists from the mix and match study are studying this, but answers will take time.
The mix and match study is one study. In epidemiology, consistency across studies is key. Unfortunately, we don’t have time to wait for more studies.
We don’t know what a “protective” level of antibodies is. So, these fold-increases may not correlate with real world effectiveness.
This study included Moderna at a 100 μg dose. This is different than what’s being rolled out (50 μg). This could influence results.
Data was only presented 29 days after original dose. J&J seems to have a delayed reaction, so this data may miss the ultimate protection that J&J can provide.
So, there is uncertainty. But overall there’s benefit to a booster and to mixing.
Risks to Mixing
It’s very safe to mix, but there are rare (but real) safety signals for specific vaccines based on age and sex:
Myocarditis and mRNA vaccines
There’ve been 2,459 cases of myocarditis reported to VAERS. This is out of 366,062,239 first and second doses of mRNA vaccine administered in the United States.
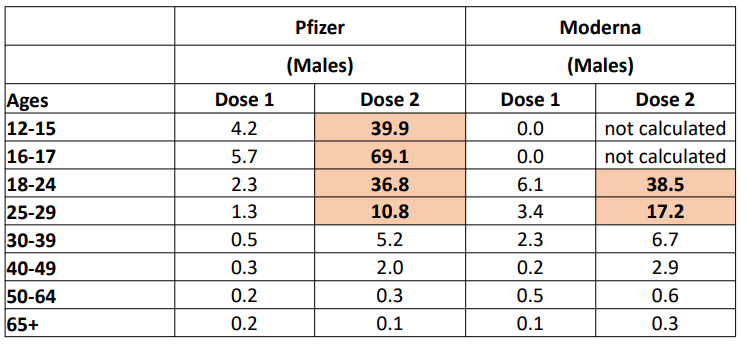
We see a higher than expected rate of myocarditis among males less than 30 years old after the second dose of an mRNA vaccine. For example, 40 cases of myocarditis have been reported out of 1,000,000 Pfizer doses among 12-15 year old males.
Myocarditis is slightly higher after Moderna compared to Pfizer (this is probably because Moderna has more RNA in it compared to Pfizer).
No deaths have been linked to vaccine-induced myocarditis. And people fully recover within 6 months.

Myocarditis data is based on the first and second shot, though. What is the risk for the third shot? We don’t really know, but this is what we’ve seen thus far…
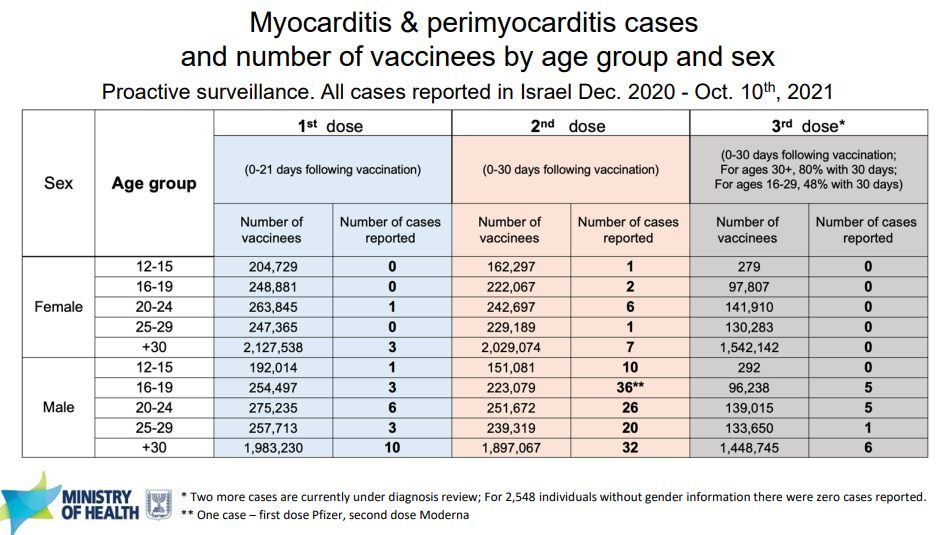
Israel has boosted 3.7 million people using Pfizer. In terms of myocarditis, a booster is less risky with the 3rd dose because of the longer period between doses. Israel reported only 17 cases of myocarditis/pericarditis after the booster. All these cases were among males.
In United States, 11,607,334 (6.1%) of people have already gotten a booster. Through the active surveillance system (V-safe), we have data on over 275,000 of those people. Most of these people did not mix, but a few people already have. For Pfizer, local and systemic reactions were reported less frequently following dose 3 than dose than the 1st or 2nd dose.

Moderna may be higher risk for myocarditis than Pfizer. But the Moderna booster is half the strength than the primary series. So, in terms of a booster, Moderna may not be more risky.
Blood clots and J&J vaccine
There’ve been 47 cases of thrombosis with thrombocytopenia syndrome (TTS—special type of blood clot) reported to VAERS after the J&J vaccine. This is out of 15.3 million doses of J&J administered in the United States.
We see a higher than expected rate of TTS among females aged 30-49 years old. For example, 11 cases of TTS have been reported out of 1,079,231 doses among 30-39 years old females after J&J.
So, what booster should you get?
The risk/benefit ratio depends on your age, sex, vaccine type, and risk for COVID19 disease. Here are some scenarios…
Young male had a primary J&J vaccine. The most protection he would get is from a Moderna booster. But there’s low risk for myocarditis with Moderna. He believes myocarditis risk outweighs high efficacy, so he goes for a J&J booster.
But maybe this guy has a comorbidity and is at high risk for COVID19 disease. In this case he wants ultimate protection. So, high efficacy outweighs myocarditis and he goes with a Moderna booster.
Middle-aged woman had a primary J&J vaccine. If she were to get a J&J booster, there is a small risk of getting blood clots. For her, a mRNA booster may make the most sense because she’s not at high risk for myocarditis. So, she goes with a mRNA booster.
But maybe she originally got J&J because she’s more comfortable with adenovirus biotechnology than mRNA biotechnology. So, for her, the minimal risk of a blot clot outweighs her concerns of mRNA.
Elderly person in rural America had a primary Moderna series, but the local pharmacy only has J&J in stock now. To them, the availability and need of a booster outweighs the small risk of blood clots. So, they will get a J&J booster.
As you can imagine, there are a million different scenarios. I hope that you can use this data to make an evidence-based decision for yourself. A conversation with your primary care provider is always a great idea too.
Ultimately, I hope we recognize how lucky we are to have access to vaccines and, moreover, a variety of vaccines. This is not the case across much of the globe.
Love, YLE
For those that missed it, I joined Dr. Beers (President of the American Academy of Pediatrics) this past Tuesday to talk about the COVID19 vaccines for 5-11 year olds. It was hosted by Scary Mommy. Here is the recording! Next week the FDA will meet to discuss the vaccine for 5-11 year olds. I’ll be in attendance and, of course, provide cliff notes.




Great news, I'm happy for everyone this helps! So this doesn't help team-mRNA people who are healthy, not in high risk jobs or living situations, without underlying health conditions? When will we hear about our booster? We know Pfizer protection wanes with time. I know I'm at less risk for hospitalization and death, but I'd also like to avoid getting a breakthrough and feeling like crap and missing work, too! My county is still purple!
Any thoughts for my 31 YO daughter who is 13 weeks pregnant. She got the J&J vaccine originally and she really doesn’t want to get the J&J booster. She is thinking about waiting until there is more data but I am leaning towards recommending the moderna booster rather than wait. She lives in TX and travels some for work so not getting booster concerns me. (her OB says get the J&J booster).